Healthy employees, healthy business: How to make a data-driven case for investing in better benefits
6 charts that show how employers can cut benefits costs without cutting corners on employee well-being


For decades, US businesses have spent more money on healthcare each year than they did the last. In part, because the healthcare system is fragmented, and patients are getting lost in the process. But some of the country’s smartest companies are discovering ways to make health benefits personalized, data-driven, and rooted in clinical knowledge. They’re bringing healthcare players together to lower their costs without cutting corners on employee well-being. These six charts prove how.
1. Employee health carries hidden costs
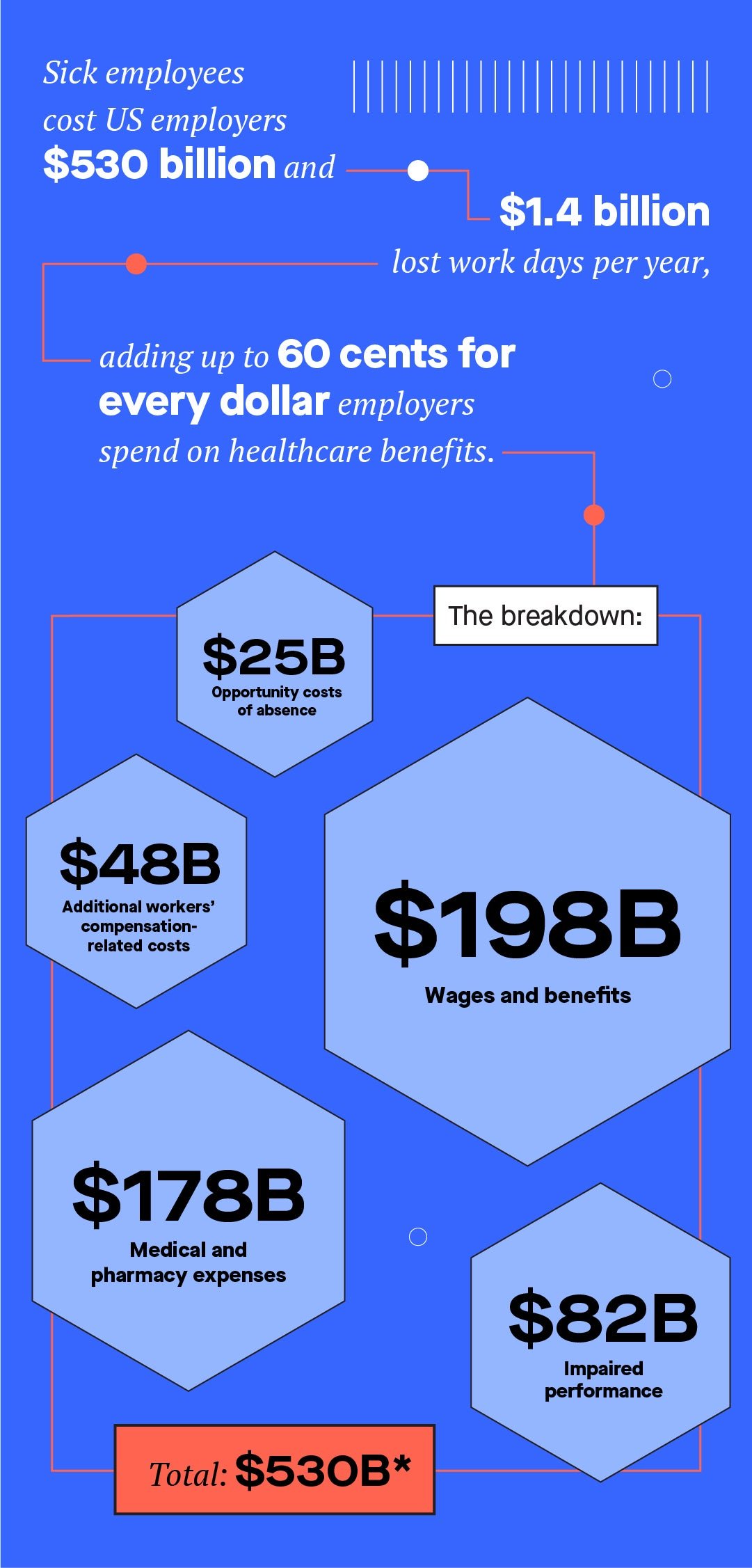
Sick employees cost US employers $530 billion and 1.4 billion lost work days per year, adding up to 60 cents for every dollar employers spend on healthcare benefits. That’s because when employees get sick and miss work, they both increase their employer’s healthcare spending and decrease their team’s productivity.
That staggering sum includes the obvious trips to the doctor and pharmacy as well as workers’ compensation and federal family and medical leave, but also the impaired performance attributed to chronic health conditions, the costs of hiring fill-in workers, paying overtime for colleagues to pick up the slack, and lost revenues in general.
2. Patients who get medication delivered to their home are more likely to take it
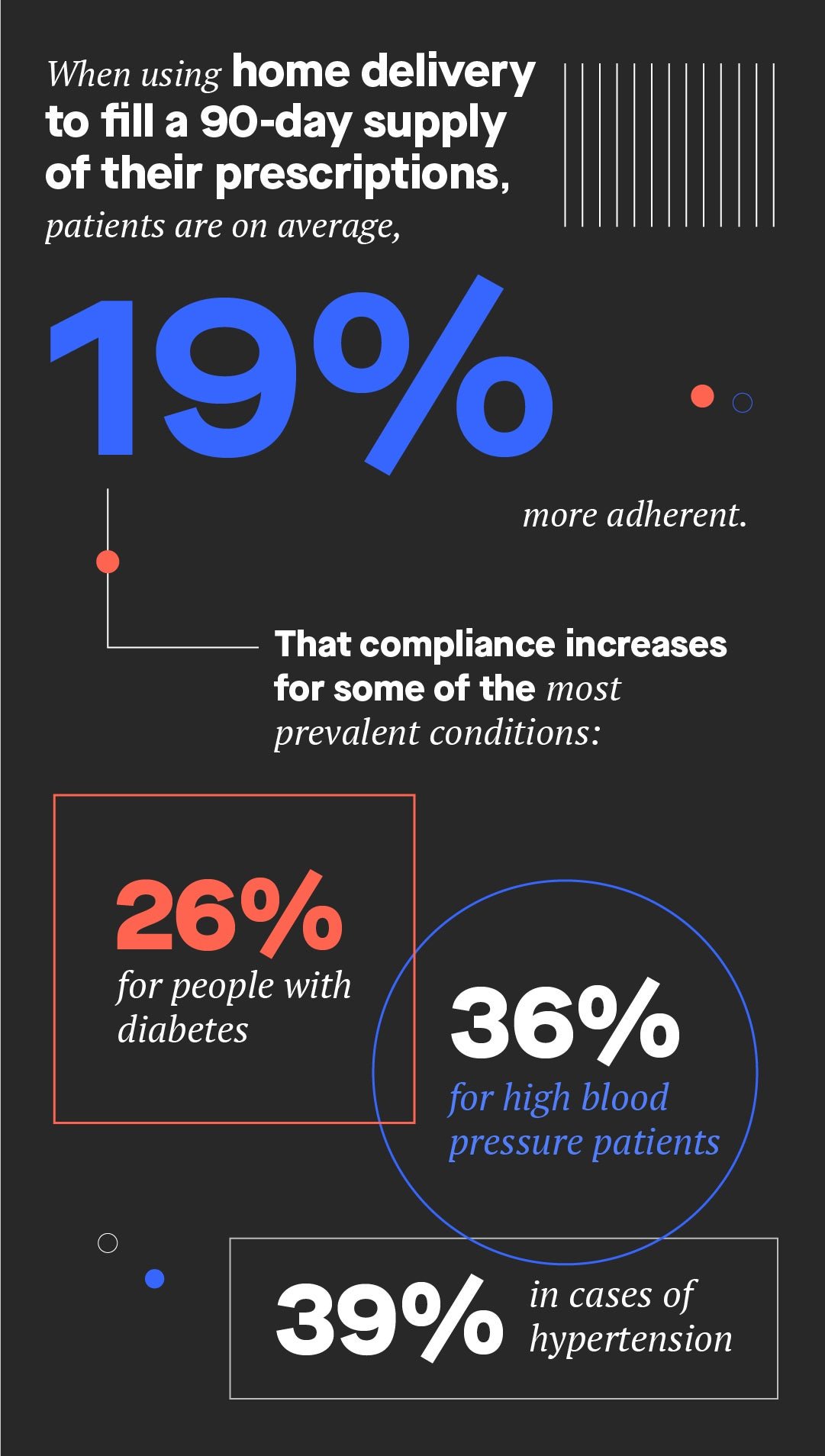
Delivering prescriptions straight to doorsteps is one of the easiest ways employers can cut costs while increasing the likelihood their employees will adhere to their treatment plans. Employers who offer home delivery pharmacy benefits can also help their employees save money: Members who use Express Scripts Pharmacy® spend 28% less on their medications than those who fill their prescriptions at traditional retail stores.
3. Patient adherence drives down healthcare costs
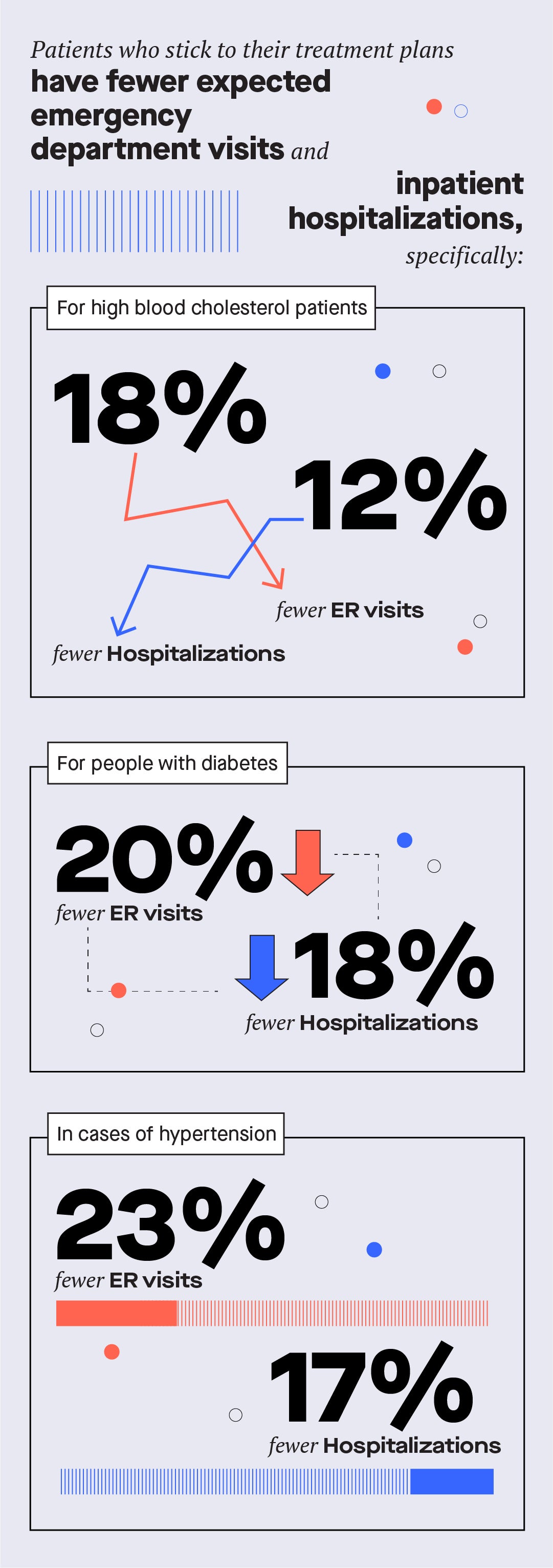
Every year, one in every nine dollars of healthcare spending is wasted because patients don’t take their medications as prescribed. In many cases, this results in costly and preventable interventions. But when patient adherence goes up, costs go down.
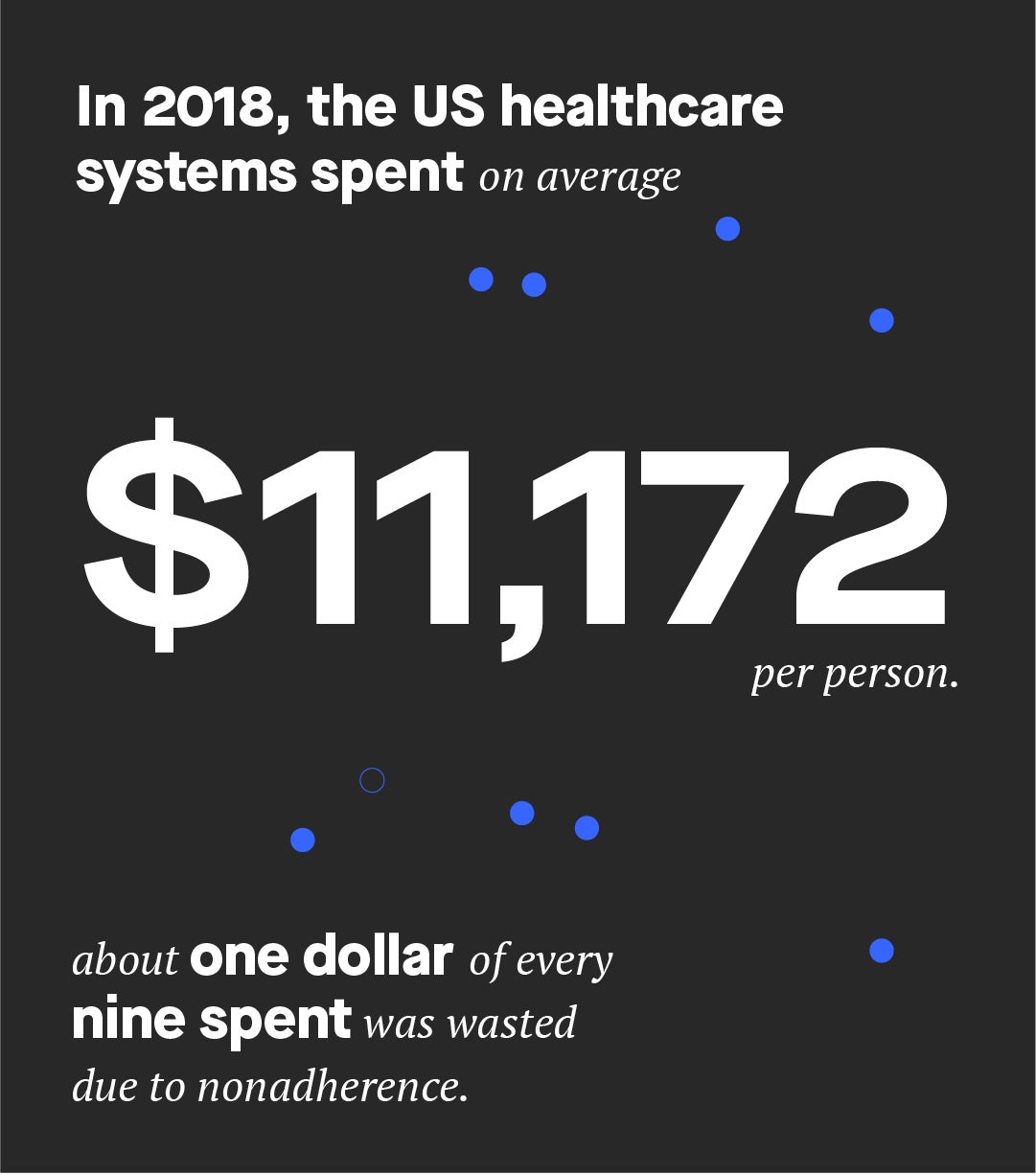
Smart businesses are relying on enhanced services like predictive analysis and digital messaging platforms to flag and remind those who need extra help for when and how to tackle their treatment plans.
4. Complex health problems are better managed when all stakeholders are on the same page
By 2030, 80 million people in the United States are expected to have three or more chronic conditions, making them more likely to need specialty medicines and more likely to end up in the hospital.

Now more than ever, it’s important for all healthcare players—payers, providers, and pharmacies—to stay in step. Connected care programs make critical data, like lab results and prescription drug claims, available at the click of a button. This holistic approach to a treatment plan helps make sure information doesn’t get lost and that everyone can see the full patient journey. Connected care also increases the likelihood that health problems are spotted sooner, reducing hospitalizations and keeping medical costs down.
5. Digital solutions empower more accessible, more integrated caregiving
The demand for digital healthcare tools has skyrocketed during the Covid-19 pandemic. In the first six months of 2020, there was a 17% increase in the number of patients using remote monitoring devices for the first time, according to M/A/R/C Research & Cigna Global Market Research and Insights. With more than 300,000 digital tools available and another 200 introduced each day, the market is ready to meet this moment.
Digital healthcare tools are the engines that make connected care possible. Remote patient monitoring leads to better chronic disease control, while messaging apps connect patients with specialists who understand their personal health needs. And there’s a clear benefit to employers, too.

Employers carry a lot of responsibility to protect the well-being of their employees, including providing the best possible health and pharmaceutical care. The most innovative businesses don’t consider healthcare as just another perk; they’re providing healthcare that works, supporting their employees exactly where they are, whether at home or at the doctor’s office.
Learn more about how these and other ways Evernorth is redefining healthcare for people and businesses.
This post is a sponsored collaboration between Evernorth and G/O Media Studios.