Fertility care has opened more doors for trans people to have biological children
When he was 22 years old, Trystan Reese wrote off having kids. He was assigned female at birth, but by that point in his life, he had realized he was transgender. He legally changed his name to Trystan, and started taking testosterone.


When he was 22 years old, Trystan Reese wrote off having kids. He was assigned female at birth, but by that point in his life, he had realized he was transgender. He legally changed his name to Trystan, and started taking testosterone.
Reese had accepted that his life would look different because he was trans. He was more likely to face discrimination, microagressions, and potentially physical violence, the stress of which put him at a higher risk of substance abuse and even early death. He didn’t know any trans people in long-term relationships, let alone those who were raising a family together. “I didn’t see that for myself,” he says. “I was moving forward for today.”
Within the next few years, though, things changed. He fell in love with his now-spouse, Biff, and through an unexpected turn of events, the couple wound up adopting Biff’s niece and nephew. As they settled into family life together, Reese found himself thinking about expanding their family even more—this time, through carrying a child.
“I truly wanted to create life…and to have that experience be a physical manifestation of this love that I never thought I’d find out in this world,” he says. “That door that had closed for me opened up again.”
Reese had been taking testosterone for over a decade, but he still had the anatomy necessary to have biological children. After going to a LGBTQ+-friendly OB/GYN clinic in Portland, Oregon, where he lived, he learned that he could safely conceive once he stopped taking his regular hormones. Biff took some convincing—he wanted kids, too, but was concerned about Reese’s safety walking through the world as a pregnant man.
Eventually, though, the couple agreed to get pregnant. They didn’t have to navigate the complex landscape of fertility care many LGBTQ+ couples have to. Biff’s body produced sperm, Reese’s body had healthy eggs, and on July 14, 2017, the couple welcomed a son named Leo.
🎧 For more intel on fertility care, listen to the Quartz Obsession podcast episode on egg freezing. Or subscribe via: Apple Podcasts | Spotify | Google | Stitcher.
Reese, who is now 37, was open about his experience while he was pregnant. He’s now the director of family formation at Family Equality, a non-profit organization based in New York that focuses on legal and lived equality for LGBTQ+ people. He’s given countless talks about his experience being pregnant and being a father, and he’s booked to address the American Society for Reproductive Medicine at its upcoming conference this fall. He hopes that by sharing his success story, he can inspire other transgender folks to realize that they, too, can conceive.
Yet he still feels overwhelmed by the work left to do for the community. These things keep him up at night, he told Quartz.
In vitro fertilization (IVF) and the fertility market that has developed around it have revolutionized the way all kinds of people can have children. In 1982, the Sperm Bank of California opened its doors to lesbian couples looking to become pregnant with the help of a sperm donor. In 1999, the first trans man gave birth in the US. That year, a gay couple living in California became the first to have both fathers’ names on their child’s birth certificate. Queer people have been having children for decades out of the public eye, but these public cases helped pave the way for future same-sex parents.
But one area of the field that has lagged distinctly behind others is fertility care for the transgender and nonbinary community, says Rafat Abbasi, a reproductive endocrinologist and infertility specialist with Columbia Fertility Associates in Virginia. Abbasi has specialized in family planning for the LGBGT+ community for nearly 30 years.
Part of the reason is a lack of representation in fertility care itself. For decades, there was an accepted belief in the medical community that taking either estrogen or testosterone to align with gender identity would render someone sterile—completely unable to have children. As a young adult, Reese assumed that he would have to make a trade between taking testosterone or having a family. When he learned that testosterone didn’t do long-term damage to his ovaries, though, he was elated. “In a world where it continues to be so difficult to survive as a trans person, one of the ways we create safety and love is through a family,” he says. “It’s one of the ways we’re able to survive, but right now most trans people think that’s not possible for them.”
More trans people are publicly out and having families of their own, inspiring others to do the same. This increased visibility is likely to prompt fertility care providers to realize that this kind of care needs to become standard. The difficult part will be figuring out how to make that care accessible to everyone.
But fear of discrimination is a big reason many trans folks don’t seek out care. A 2014 survey by Lambda Legal, a non-profit law firm that works exclusively in LGBTQ+ rights, found that 70% of trans patients had experienced serious discrimination in a doctor’s office. This fear is heightened when it comes to dealing with issues of fertility, which often bring up the gender that someone was assigned at birth.
“Between dysphoria and sort of the general cultural stigma…historically family building wasn’t really something that they were thinking about as an option,” says Signey Olson, a nurse practitioner and nurse midwife who also works at Columbia Fertility Associates out of their Washington, DC office. (Signey uses both she/her and they/them pronouns.)
Fortunately, there have been some providers who have always catered to these communities. These groups—most of which the community finds through word of mouth, Olson says—have collectively worked to establish some of the baseline levels of care for trans and queer folks, like Columbia Fertility Associates. By providing inclusive fertility care, they’re setting the standard for how care should look for everyone.

The biology at hand
The way that fertility care should start for the trans community is the same way it starts for anyone: with dignity. Providers should recognize and include both partners equally, and make sure that they immediately use everyone’s chosen names and identities—even if they differ from their legal names—as they move in and out of the office.
Beyond that, “the science of this is straightforward,” says Mark Leondires, a reproductive endocrinologist and medical director and at Reproductive Medicine Associates of Connecticut and Gay Parents To Be.
To have a biological child, all you strictly need is a pair of matching gametes: a spermatocyte and an oocyte. Most forms of transition—excluding some surgical options—don’t affect those baby-making cells.
When trans people come for fertility care at a place like Columbia Fertility or the Reproductive Medicine Associates of Connecticut, they’re either currently on estrogen or testosterone, or are considering hormones. When a trans woman takes estrogen or a trans man takes testosterone, they often can’t produce a biological child. (Although it can happen—it’s one of the few cases in which a queer couple has an accidental pregnancy, Leondires says.)
“Option one is to freeze eggs or sperm, if you can do it financially and emotionally, and fits into everyone’s timeline,” Leondires says. Of course, that would mean delaying transitioning a little bit longer.
Many trans people, like Trystan Reese, have already begun taking hormones by the time they decide they want to try to conceive. For Reese, this deciding moment was a distinct one: One day, when he was carrying his newly adopted daughter, Biff’s biological niece, around the house, she had a bout of diarrhea that soiled them both. Without thinking, he stripped them both down and got into the shower.
At that moment, he realized he was already in the thick of fatherhood. The idea of being a biological parent, which he had quelled about a decade ago, stirred.
He began doing research, fervently. “I was most concerned about the medical aspects of it,” Reese says. As a self-described nerd, he created a meticulously curated Google Drive folder of all the scientific literature he’s collected over the years, starting with when he decided he wanted to become pregnant. “I didn’t want to do anything unsafe for the baby,” he says.
Assuming a trans man has no underlying health issues, and is under 38 (the age at which risk of miscarriage increases), to become pregnant, all they have to do is stop taking testosterone. Within six months on average, their ovulatory cycle will resume. If their partner produces sperm, and both parties are otherwise healthy, they can get pregnant the old-fashioned way—that’s how Reese got pregnant nine months after he went off testosterone. If either are having fertility problems or both have ovaries, the couple can think about using a sperm donor and elect intrauterine insemination (IUI) or IVF.
During conception and through pregnancy, trans men can’t take testosterone—which can be daunting. “I was willing to go through the trials of going off hormones, regaining an ovulatory cycle, having my body change and shift in a way that would be perceived as being more feminine,” says Reese. But that may not be the right choice for everyone. If it isn’t, this is where surrogacy may be an option, though it is more expensive.
Going off testosterone may not lead to drastic physical changes. “Many people get most of the effects they’re looking for after two years,” including a more defined jawline and facial hair, says Olson. “There isn’t usually a reversal of most of those.” For better or for worse, a lot of trans men get asked if they have been gaining weight.

Trans women should be able to start producing sperm again once they stop taking estrogen and other medications that block testosterone, too. A small study published last year showed that as long as individuals taking estrogen stopped about four months before providing a semen sample, their sperm were normal. Like with testosterone, the physical effects of taking feminizing hormones for multiple years shouldn’t revert after a short period of time off of them.
That said, this is one of the areas where research is lacking. “We just don’t know very much,” says James Smith, a urologist at the University of California San Francisco who co-authored the paper. Smith is the director of male reproductive health in the department of urology at the University of California San Francisco. He works with cis men who are taking testosterone and transgender women who are taking estrogen who want to conceive children. There’s still no good data on the long-term effects of taking estrogen on sperm production, so right now he uses the same guidelines for both groups: wait three months before providing a semen sample.
That said, it’s different for everyone: He’s also encountered patients who have discontinued estrogen for months and still been unable to produce normal sperm. It may not be the result of the estrogen: They could have had fertility issues their entire lives. But without a baseline count, or more research in the field to back it up, it’s impossible to know.
In cases where there may be problems with the sperm, clinicians can offer traditional fertility care methods—in the case of a lack of swimming sperm, intracytoplasmic sperm injection, or ICSI, may be an option, assuming the couple also has access to eggs. These struggles are the same as what some cis men and women’s face with infertility, and fortunately, ICSI works about 80% to 90% of the time.

Beyond biology
For anyone, there’s so much more to fertility care than the biology itself. For trans folks in particular, the emotional component may be a significant hurdle to clear.
“It’s really hard to understand your sexuality and your gender identity,” says Leondires. Once someone figures that out for themselves—and knows they want a child in their lives—they have to prepare all over again for the changes to their body if they have to discontinue gender-congruent hormone use.
That’s why the best fertility care teams for trans folks include both clinical and mental health support—and possibly a reproductive attorney if there are gamete donors involved, Leondires says. Lawyers ensure that partners are legally recognized as parents of their child, even if their DNA wasn’t involved. “The hurdles are higher than, let’s say, a cis-gender woman with a female parter, or a cis-man with a male partner,” he says. “But they are surmountable.” His own practice at Reproductive Medicine Associates of Connecticut employs a social worker to help people navigate some of the emotional aspects.
Health care settings can also help parents feel safe by making small, conscious changes to their practice. “‘Vagina’ is not something that [many trans people] associate with that part of their body,” Olson says. Instead of calling a procedure a “trans-vaginal ultrasound,” it may be better to refer to it as a pelvic ultrasound or internal ultrasound—it depends on what the person is most comfortable with.
Practices like this are extra important when it comes to giving birth. At these moments, when individuals or couples are most vulnerable, micro and macro aggressions can make an already stressful process even worse.
“Labor and delivery wards are very feminized,” says Madeline Deutsch, a primary care specialist and the director of transgender care at the University of California, San Francisco. “The rooms are pink, the gowns are pink, the language is gendered—it’s hard-wired.” After birth, other hurtful oversights can occur: Listing someone as a “mother” instead of a parent on a birth certificate, or failing to acknowledge someone’s partner as such. These aggressions can trigger a flood of memories of abuse and discrimination. “Trauma is like a bruise,” Reese says. You don’t have to hit it very hard for it to hurt.
Fear about treatment in hospital settings greatly skews where trans men choose to give birth. A study published in 2014 (paywall) reported that 22% of trans men choose to give birth in places other than a hospital. In the cis community, that figure is around 1.28%. The same study found that 23% of trans men elected to have either a lay midwife or no prenatal care, choosing to avoid a formalized medical setting altogether—which could be dangerous if complications arise during childbirth.
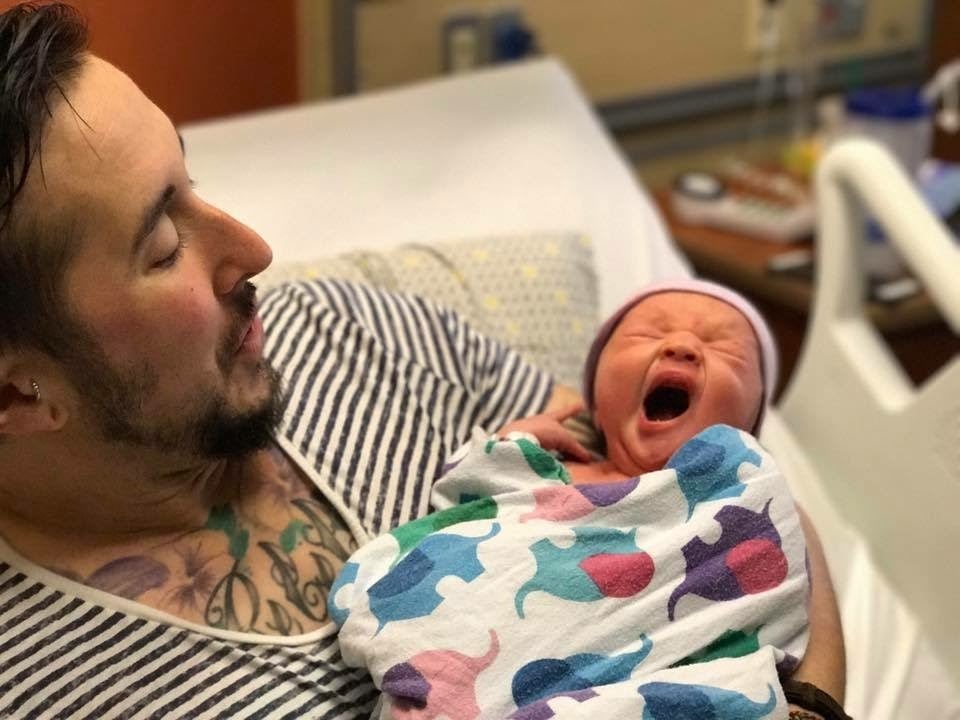
Trystan Reese ended up giving birth in a Kaiser Permanente Hospital in Portland. “You get whatever midwife is there,” he says. And even though he had an okay experience with his birth, he said he still felt like he had to give some feedback to the staff. An ultrasound technician misgendered him, and the lactation consultant wasn’t equipped to deal with two men having a baby together. Because of his work, Reese felt comfortable advocating for himself and speaking up—but not all trans people may feel that way.

Improving care
Because the transgender community constitutes less than 1% of the total population, medical settings don’t get a ton of experience treating trans folks. And unfortunately, the same pattern exists in research communities, which is critical to improving fertility care.
There’s essentially no data on what happens to men who give birth as they go through postpartum changes. About one in nine cisgender women experience postpartum depression; preliminary work suggests that trans men are at an even higher risk, which may or may not include bouts of gender dysphoria.
Another glaring void in research is whether or not trans kids will be able to preserve their fertility if they transition using hormones before they hit puberty. Reese transitioned after he had gone through puberty, so his ovaries had the chance to mature with the cascade of hormones that puberty brings. But as kids gain support in expressing their gender identity, some will forgo puberty, taking gender-congruent hormones before they develop secondary sex characteristics like voice dropping or breast development. And researchers don’t know what this may do to long-term fertility.
Without going through puberty, sperm production and eggs may not develop typically. Right now, Smith’s clinic at UCSF and a clinic at the University of Pittsburgh will take testicular and ovarian tissue biopsies and freeze those tissues, in the hopes that one day, the science will advance enough to coax these tissues into producing mature gametes in the lab. There have been animal models and some evidence that this is possible in cases where pediatric cancer patients have tried to preserve their fertility before undergoing treatment. But these data have come from case studies—not larger research papers.
“Many trans adolescents take hormones and puberty suppressants that are life saving,” says Reese. “I just wish we had more options to allow transgender adolescents to access live saving treatment while also preserving their future fertility.”
The big thing that he focuses on now is that in the US, fertility care is getting better for trans folks, slowly but surely. Through his work at Family Equality, Trystan has designed a three-hour digital course for health care providers who are interested in becoming more LGBTQ+-friendly. The more centers that can provide trans folks with a good experience, the more people will flock to them.
Ideally, the visibility among the trans community can then show others that it’s possible to have the kind of love that manifests itself in children. “That was my light,” says Trystan. “I followed that through the ups and downs.” Now, Trystan and Biff’s son Leo is two-and-a-half years old. “He’s just started saying ‘I love you, Daddy,’” Trystan says. “Those moments are just unrestrained desire and connection and love, and I want that for everyone who wants that.”