How long will Covid-19 vaccines protect you from infection?
The first Covid-19 vaccines from Pfizer and BioNTech are being distributed in the UK this week, marking a turning point in the pandemic. As more countries move to authorize and disseminate vaccines, the end of the pandemic can feel tantalizingly close. But before we can get a clear idea of when and how life could return to normal, we have a number of outstanding questions to answer.
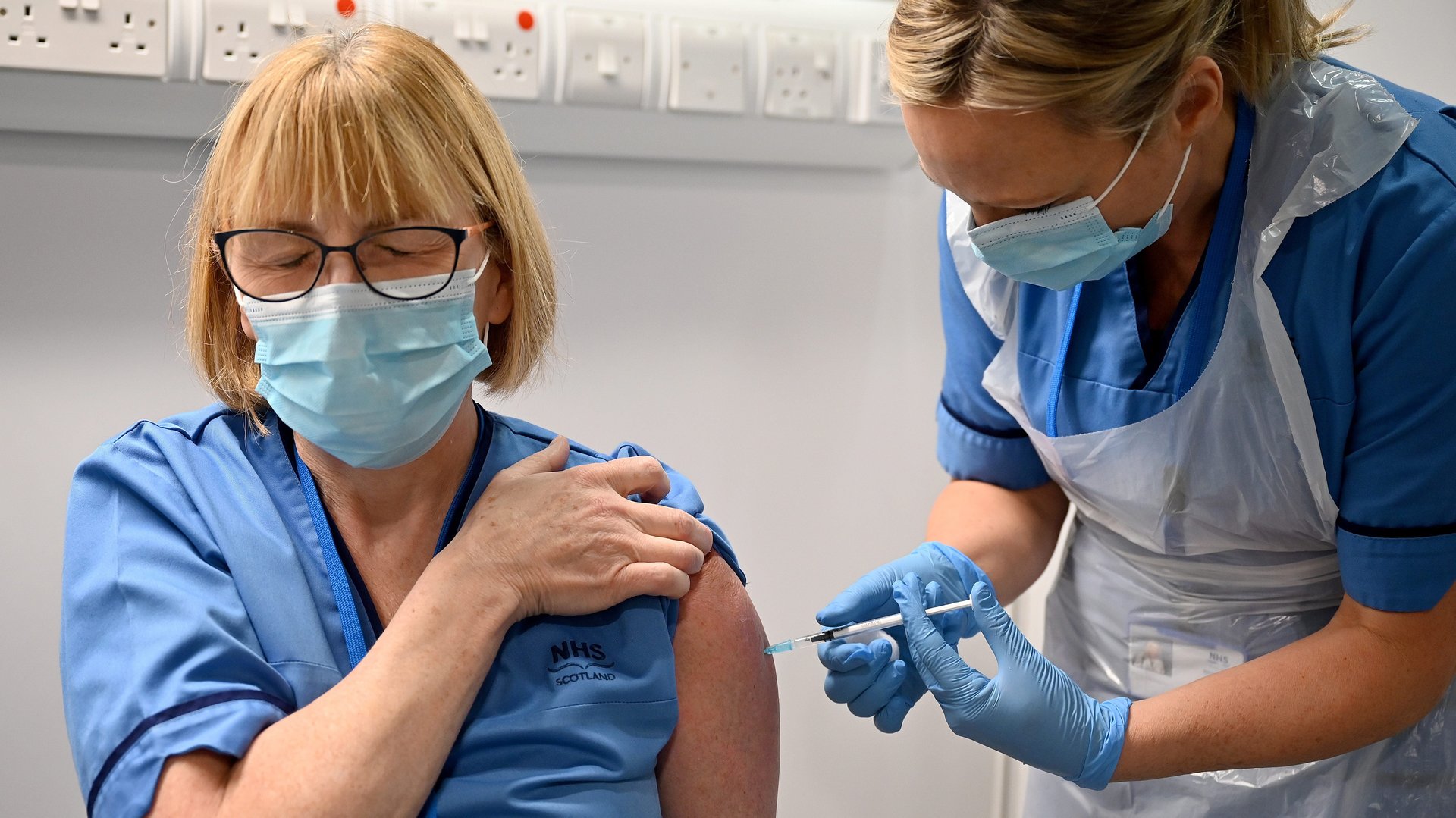

The first Covid-19 vaccines from Pfizer and BioNTech are being distributed in the UK this week, marking a turning point in the pandemic. As more countries move to authorize and disseminate vaccines, the end of the pandemic can feel tantalizingly close. But before we can get a clear idea of when and how life could return to normal, we have a number of outstanding questions to answer.
One of those remaining unknowns: Once an individual is vaccinated, how long will their immunity to Covid-19 last? To answer this question and others, scientists need to collect more data from vaccine trials—some of which will simply take longer to collect.
At the moment, only three vaccine candidates—those from Pfizer and BioNTech, Moderna, and AstraZeneca and the University of Oxford—have released meaningful safety and efficacy data from their late-stage clinical trials. These data are enough for global regulatory bodies to assess whether or not to authorize the vaccines for widespread use. But every Covid-19 vaccine in the pipeline will continue those trials well beyond authorization.
The question of the duration of a vaccine’s efficacy “will be part of ongoing studies,” Albert Bourla, the chief executive officer at Pfizer, said on a press call with the International Federation of Pharmaceutical Manufacturers and Associations on Dec. 8. The answer doesn’t just depend on how a vaccine performs; it could also change depending on how SARS-CoV-2 acts in the real world.
Early evidence from individual cases has suggested that it’s possible to develop Covid-19 more than once. Scientists still aren’t clear on why this happens; theoretically, after we get sick, our immune cells should build up antibody defenses that will be ready to tackle future infections even faster. It could be that Covid-19 is more like seasonal viruses, like the cold or flu, for which we don’t retain long-term immunity. In that case, beating back the pandemic and keeping it back would require repeated vaccinations.
Cold and flu viruses also mutate substantially year after year, which is why we need flu shots annually; there is no vaccine for the viruses that cause the common cold. In that case, we might have to redesign the Covid-19 vaccine before we take it again. But so far, it seems like SARS-CoV-2 is spreading faster than it mutates—which means that we likely won’t need new vaccines every year.
It could also be that reinfections simply occur when individuals didn’t get sick enough to develop strong antibody responses against the virus. If that’s the case, there’s a chance vaccines could generate a stronger immune response than these weaker cases, protecting people for multiple years. Early mouse studies of mRNA vaccines targeting SARS-CoV-2 provided immunity to mice 13 weeks after they received two doses, which could translate to years of time in humans.
But the fact remains that no one really knows the answers to these questions. Scientists will just have to keep collecting information from the continued vaccine trials to know for sure.
The Pfizer/BioNTech and other trials will extend for dozens of months. Tens of thousands of trial participants will continue to check in periodically with healthcare providers, providing more data about long-term safety and efficacy and receiving supportive care should they need it. If participants who received the vaccine go on to develop Covid-19 after a year, for example, scientists will know that annual boosters may be necessary.
These long-term follow ups can answer other remaining questions about Covid-19 vaccines, too. They can assess if vaccine candidates actually stop viral transmission, or if they only protect individuals from getting sick. (Theoretically, vaccines should stop transmission as they eliminate the chance for the virus to replicate inside us.) They’ll also be able to demonstrate any long-term side effects from these vaccines.
As this information becomes available, it can help inform public health decisions about re-opening schools, restaurants, or unrestricted travel. But until we have a complete understanding of both the virus and the vaccines that protect against it, basic public health tools—tracking local transmission and hospitalization rates—are one of our best weapons.