A shocking number of US nurses are quitting, but a majority would stay for more money
The US is losing nurses when it needs them most. The nurse shortage that began prior to Covid-19 was exacerbated by the pandemic burnout and is already compromising some hospitals’ ability to provide care.
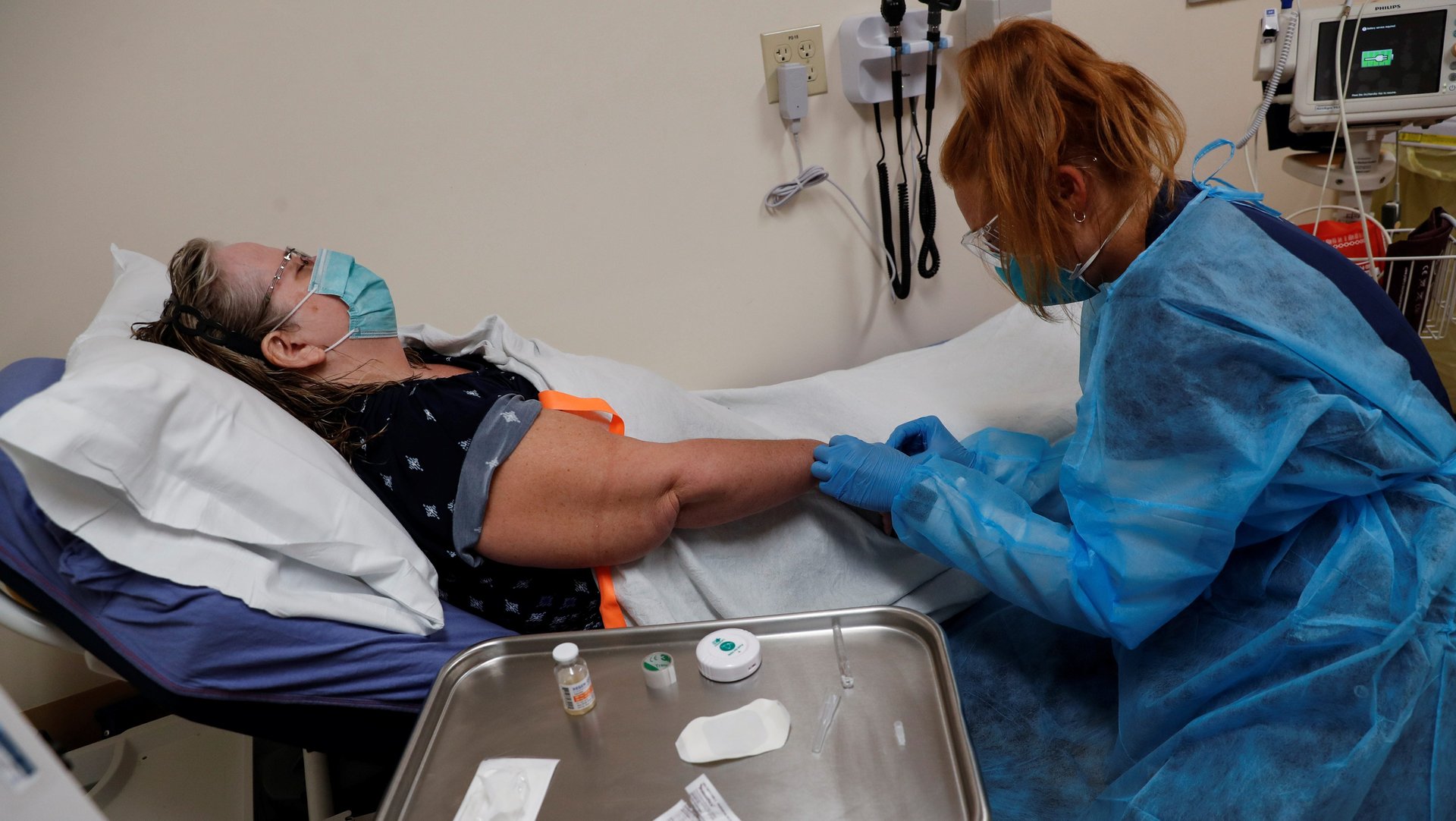

The US is losing nurses when it needs them most. The nurse shortage that began prior to Covid-19 was exacerbated by the pandemic burnout and is already compromising some hospitals’ ability to provide care.
A recent estimate by Mercer, a healthcare consulting firm, estimates more than a million nurses will leave the workforce by 2026, while demand will keep rising, leaving providers in most states in dire straits. California and New York are both expected to face a shortage of more than 500,000 nurses.
Last week, US president Joe Biden’s administration announced a plan to invest $100 million to support states in training, recruiting, and retaining healthcare workers, particularly for rural areas. While a step in the right direction, the program will take time to make any significant dent, and hardly help with the one intervention likely to keep nurses in their jobs: higher salaries.
It isn’t all about higher pay—but it helps
A survey by ShiftMed, a healthcare staffing agency used by 60,000 nurses, found that 49% of its nurses are somewhat likely to quit the field in the next two years.
Overall, 76% of nurses said they felt the desire to help others wasn’t enough to keep them in the job, and they are looking at other benefits to remain in a profession where, according to the survey, they feel unsafe, at risk of burnout, and mistreated.
Relatively simple professional adjustments would help retain nurses, the survey found, including more paid time off, flexible schedules, a more cooperative environment, and better shifts. But the two incentives most commonly cited as motivators to stay wouldn’t be quite so easy for hospitals and other facilities to provide: more staffing, and better pay.
Nearly 60% of nurses said they would not leave their jobs if they had higher salaries, and nearly as many (54%) said they would stay if their workplace had a larger staff, which would allow for better shifts and higher quality of care for patients.
Increased staffing isn’t easy goal to provide in the current shortage, nor is higher pay. This is especially true for independent hospitals in rural areas, which often lack the financial resources to hire more staff, or keep up with climbing salaries.
How much does a nurse make?
Nurse wages vary dramatically depending on their roles, ranging from a national average of about $31,000 for assistant nurses to $181,000 for nurse anesthesiologists. But salaries are very different according to the state, too. In Mississippi, a registered nurse made on average just under $60,000 a year in 2019; in California, the average pay was more than $113,000.
As shortages become more critical, however, an increasing number of nurses are leaving full-time jobs that pay regular wages to join staffing agencies such as ShiftMed. The agency brokers shifts with 1,000 hospitals around the country, connecting nurses—either freelance or those interested in extra shifts—with hospitals with staffing shortages. Through a service such as ShiftMed, hospitals compete with one another to attract talent to fill the increasing staffing gaps, and to do so they have to offer competitive arrangements—starting with wages. A hospital trying to attract a nurse from out of town can spend as much as $9,000 a week.
“For the first time ever, nurses have the power to choose,” says Todd Walrath, the CEO of ShiftMed, noting that the current shortage of at least a million nurses gives the ones who are staying in the profession the upper hand. Platforms like his give nurses a chance to compare shifts and perks, selecting the jobs and shifts that most closely align with their professional and life ambitions.
Offering this kind of flexibility—or better benefits overall—can improve the quality of life of nurses and stop them from leaving the workforce. But it doesn’t really help reduce the shortage, since it just shifts the limited number of nurses from one hospital to another. It also drives up the costs of administering healthcare in a way that isn’t sustainable for many providers. Not only are rural hospitals struggling to compete with wealthier competitors to attract new nurses, but they risk losing their own staff to those offering better wages.
This kind of dynamic is likely to continue, if not worsen, for as long as the shortage persists. “I don’t know if there is a solution for a standalone rural hospital that can’t afford to pay higher rates,” says Walrath.