We still don’t know what to do with women who have “stage zero” breast cancer
A cancer diagnosis in any form is scary. So what does it mean when you’re told you have “pre-cancer” of the breast? The truth is, even doctors aren’t exactly sure.
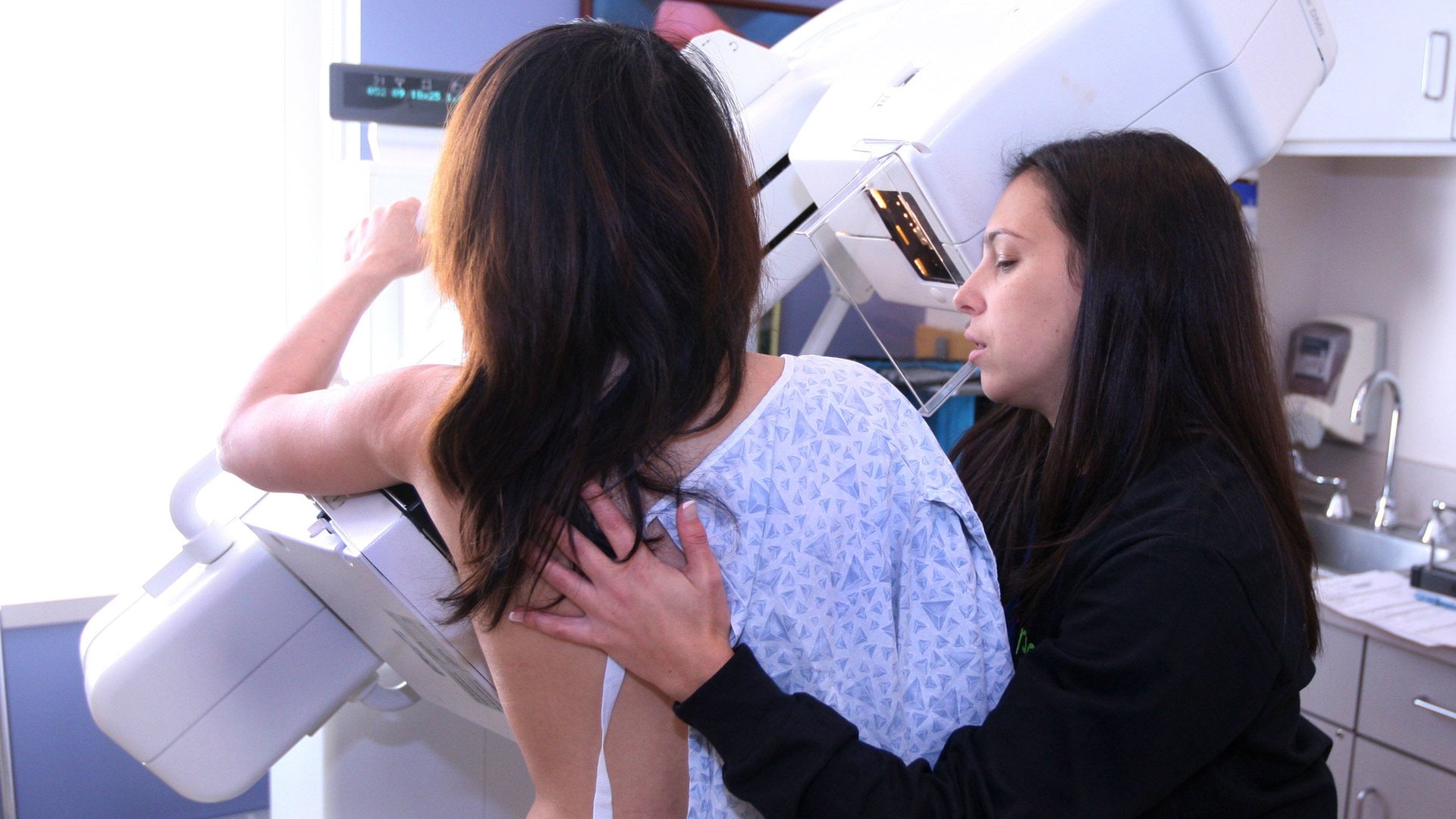

A cancer diagnosis in any form is scary. So what does it mean when you’re told you have “pre-cancer” of the breast? The truth is, even doctors aren’t exactly sure.
But a massive new study has the medical community rethinking its approach to treatment, and has led to questions about whether thousands of women are undergoing unnecessary surgery and radiation treatment.
The “pre-cancer” in question is called ductal-carcinoma in situ (DCIS), and it denotes the presence of atypical cells that have not yet left the milk ducts. DCIS is considered “stage zero,” but the oncology community has not reached consensus on what exactly DCIS is, and whether it should be considered a cancer, a precursor to cancer, or simply a risk factor. For many women, tumors never advance beyond their initial occurrence, in situ.
Nearly a quarter of all new breast cancer diagnoses in the US are for DCIS, and the number has been increasing both because of more screening and the fact that women are living longer. Traditionally, DCIS is nearly always treated with a combination of radiation and a lumpectomy (in which the tumor and some surrounding tissue are removed) or a mastectomy (which removes the whole breast) or double mastectomy.
But a new study from JAMA indicates that such treatments do not affect the mortality rates of women who have DCIS. JAMA examined data on 108,196 women in the US—almost all of whom had had either lumpectomies or mastectomies—and found that they still had a 3.3% chance of dying of breast cancer in the two decades after treatment, similar to women without the diagnosis or treatment. The risks were higher for black women and women who were diagnosed before the age of 35 (the mean age in the study was 53.8).
“Given the low breast cancer mortality risk, we should stop telling women that DCIS is an emergency and that they should schedule definitive surgery within 2 weeks of diagnosis,” writes Laura Esserman of the University of California, San Francisco in an editorial accompanying the study. Instead, she writes, “Much of DCIS should be considered a “risk factor” for invasive breast cancer and an opportunity for targeted prevention.”
But as I’ve written before, death is not the only consideration when dealing with cancer. Even survivors have to live with the fear of recurrence and the trauma of a lifetime of treatments. Each patient has her own unique medical history, set of genes, type of cancer, and risk factors. It’s likely that genetic testing and more targeted tumor tests will help doctors and patients make more personalized decisions about how to treat DCIS. But we still don’t really understand how these lesions will behave. And to categorize DCIS as non-cancer, or not requiring treatment, is dangerous—especially since the authors do note that treatment reduces the risk of getting an invasive form of breast cancer.
The researchers find:
Only a fraction of treated DCIS lesions progress to invasive breast cancer, but in the absence of treatment, the risk of invasive cancer is much higher. Also, mortality from breast cancer in women with DCIS increases substantially following the development of an invasive local recurrence.
And, one of the most surprising findings of the study was that women who died from DCIS (54% of deaths in the study) did not have invasive breast cancer before presenting with metastatic cancer. Breast cancer can recur in the liver, lungs, bones, and brains (as well as lymph nodes). This means that DCIS on its own can be deadly.
While it’s important to remember that those cases don’t make up the majority—80% of DCIS is low-risk—you certainly wouldn’t want to be treated with a one-size-fits-all approach if you were part of this cohort.
Several doctors told the New York Times (paywall) that they wouldn’t revise their treatment plans until randomized trials are performed to compare the outcomes of no treatment with those of non-invasive hormonal therapies or surgery.