Zika is a warning to the US public health system to stop rushing from fire to fire
With mosquito season looming in the US, health officials expect to see Zika virus infections rise this summer. The disease, transmitted by Aedes mosquitoes, was definitively linked by the US Centers for Disease Control and Prevention (CDC) to the birth defect known as microcephaly last week.
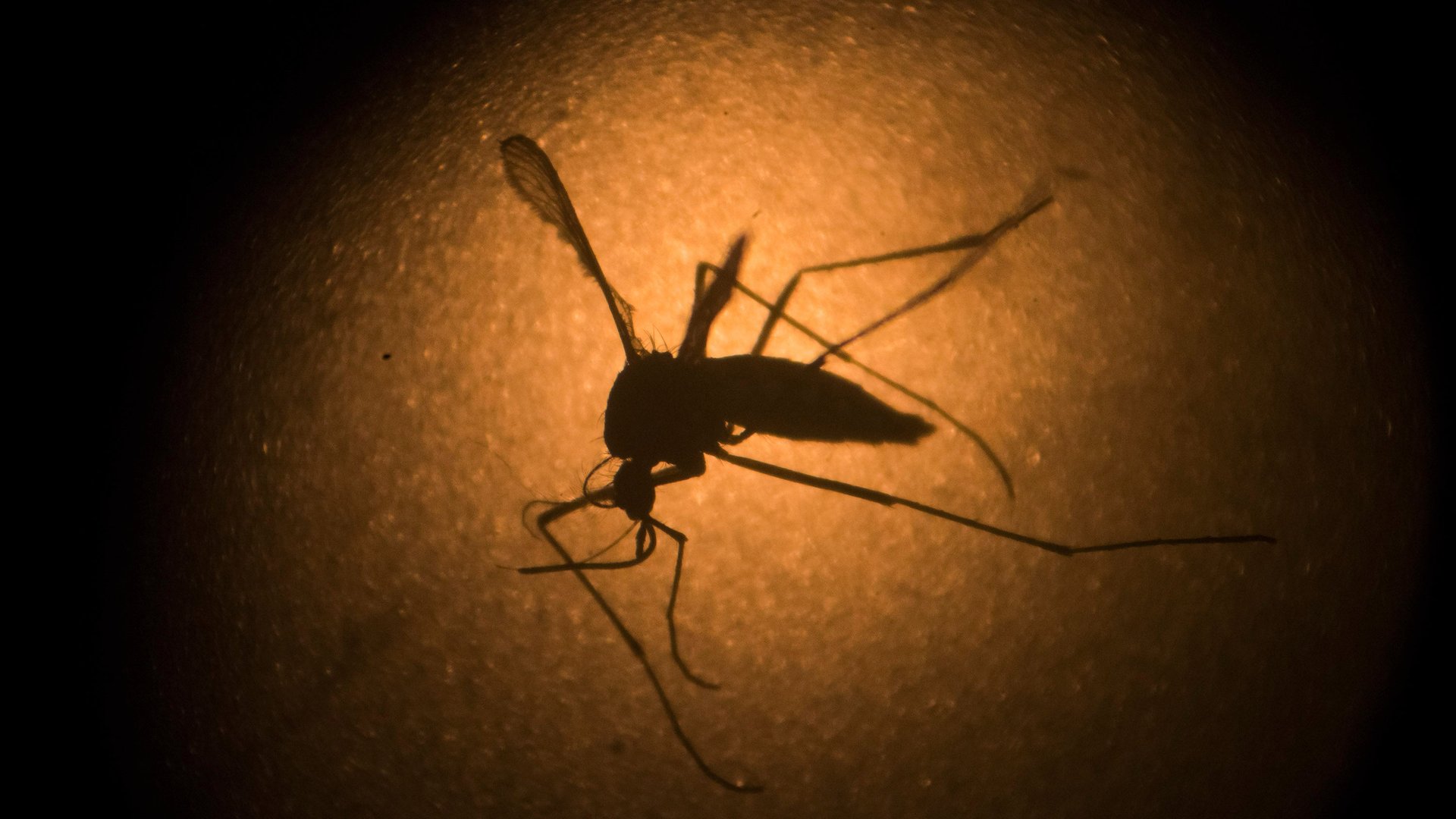

With mosquito season looming in the US, health officials expect to see Zika virus infections rise this summer. The disease, transmitted by Aedes mosquitoes, was definitively linked by the US Centers for Disease Control and Prevention (CDC) to the birth defect known as microcephaly last week.
The Obama administration has wisely shifted funds to kick-start the national fight against Zika in advance of the summer. But the government’s struggle to come up with sufficient money to battle Zika without compromising other public health efforts has exposed all that’s wrong with the US approach to health security.
In February, the White House requested more than $1.8 billion in emergency funding to stop Zika transmission. Congress has yet to act on this request, deferring a decision to its annual budget battle in the fall. So the Obama administration temporarily shifted $598 million—almost all from unspent Ebola funding—to Zika control.
But it makes no sense to choose between fighting Zika or Ebola. While it’s true that Ebola is no longer classified as an international public health emergency, it remains a real problem. In recent weeks, it’s flared up in both Guinea and Liberia, likely because of transmission by male survivors. And as the CDC notes, while Ebola outbreaks are unlikely to occur on a large scale in the US, it’s important to have systems in place that allow us to prevent this and other epidemics.
What the Ebola epidemic should have taught us is that it’s important to have surveillance for disease outbreaks in place, as well as stronger local health systems to respond when they occur. The conditions that led to the Ebola outbreak in the first place—weak health systems, unsafe water, lack of hygiene and sanitation—remain largely unchanged. We can’t just keep running from one fire to the next, whether the current most pressing threat is Zika, Ebola, Legionnaire’s disease or lead in the water supply.
Yet historically, there’s been little long-term political will to sustain public health funding. Cuts to tuberculosis control programs in the 1970s and 1980s led to a resurgence of the disease a decade later, costing New York City alone over $1 billion. The threat of bioterrorism spurred increased funding for public health emergency preparedness in the wake of 9/11, but this has been cut by more than a third over the last decade. Since 2002, CDC funding to support state and local efforts to monitor and control mosquito- and tick-borne diseases was cut by 74%. Meanwhile we’ve seen the spread of West Nile virus and the emergence of dengue and chikungunya in Florida, Texas and Hawaii.
On a broader level, public health, which is charged with health security, is chronically underfunded. It accounts for less than 5% of total health-care spending in this country, and is suffering more cuts even as our spending on medical care grows. We spend more on administrative overhead for medical services than on public health. And since the recession of 2008, over 50,000 state and local public health jobs—about one-fifth of the workforce—have been lost.
Public health funding remains inadequate and unreliable largely because of its convoluted funding structure, which relies on federal, state and local funding streams. Federal funding draws from personal and corporate taxes, while state funding comes from sales and excise taxes, and local funding is derived from property taxes. Each of these budgets is determined on an annual basis, and is therefore inherently unstable. That makes it very difficult to form long-term strategic plans for disease prevention and control, especially when public health programs already have to make do with so little.
Moreover, because wealthier states, cities and counties have stronger tax bases, differences in public health spending are often quite wide. In 2013-2014, for example, median per-capita state spending on public heath was $31.06 (remember that much of this comes from the federal government), ranging from $3.59 in Nevada to $156.01 in Hawaii.
On the local level, in 2005 (the latest data available), public health spending was more than 13 times higher per capita in the top 20% of communities versus the bottom 20%, even after taking into account differences in demographics and types of services provided. But when you’re fighting diseases like Ebola or Zika, you’re only as strong as your weakest link. So no matter where you live, you should be personally concerned when poorer communities don’t have the resources they need to, say, control mosquitoes this summer.
We know that higher levels of local public health spending translate into lower rates of preventable disease and death. So in the face of tighter budgets, how do we ensure adequate, stable funding for public health?
Some have proposed national excise taxes on medical services, health insurance or unhealthy products like sugary beverages. Excise taxes are folded into the price of a given product, such as fuel, alcohol, cigarettes, plane tickets or the like—and tend to support a related service. The federal Highway Trust Fund, for example, is funded by excise taxes on fuel.
Alternatively, some of the Medicare trust fund could be allocated for public health. Others have suggested permanently extending the federal estate tax and directing the funds to public health. Estate taxes are an attractive option for public-health funding because higher rates are unlikely to have much impact on economic productivity.
The deeper issue is that since the wealthy can often shield themselves from public-health crises, up to a point, the political will to make such changes just isn’t there. With Zika, the people who pay the price are often the poor: their homes are most likely to lack air conditioning or window screens, and they’re most likely to live close to the trash heaps and standing water that attract mosquitos. Moreover, poor women have less access to contraception and so are more likely to be the ones with pregnancies affected by Zika.
Of course, if Zika really takes hold, even the most privileged will have limited options to protect themselves from the infectious disease. How bad will things need to get before we take seriously the need to fund public health?