Why is Africa’s Covid-19 vaccination rate so low?
As the new, highly mutated omicron drives a fourth wave of infections in South Africa, countries around the world are wondering what the variant will mean for lives and economies. They need only look at what’s come before.

As the new, highly mutated omicron drives a fourth wave of infections in South Africa, countries around the world are wondering what the variant will mean for lives and economies. They need only look at what’s come before.
Scientists caution the world will always remain at risk of new, more mutated variants so long as rich countries continue to hoard vaccines. That should make vaccinating Africa a priority.
Almost a year after Covid-19 vaccines became available, more than 80% of Africa’s population have not seen a single dose of a Covid-19 vaccine, says Dr. Abdou Salam Gueye, emergency director with the World Health Organization’s (WHO) regional Africa office. “Only about 102 million Africans, or 7.5%, of the continent’s population is fully vaccinated.”
By comparison, about 60% of the general population in the US are now fully vaccinated, and this proportion climbs to nearly 70% in the UK. In Canada, and Japan, two-thirds of the general population is fully inoculated against SARS-CoV-2. Booster shots are becoming widely available in all four countries.
Rich countries were able to get ahead by securing almost twice as many Covid-19 vaccines as Covax. The vaccine distribution network was intended to be the world’s mechanism to ensure poorer countries, most of them in Africa, weren’t left behind.
Wealthy nations secured the “lion’s share” of jabs before any had even been shown to work, Mohga Kamal-Yanni, a UK-based expert in global health policy and access to medicines has explained. Pre-Covid, the world typically produced about 4 billion doses of any vaccine annually. By September 2020, before any Covid-19 vaccines had been approved for use, just five economies—the US, the UK, Canada, the EU, and Japan—had already secured deals for an estimated 4 billion possible doses of frontrunner vaccines.
Without access to jabs for much of the coronavirus pandemic, vaccination campaigns in Africa started months behind countries such as the US. Now, the continent is racing to catch up.
Africa’s problem is of vaccine supply, not vaccine hesitancy
Wealthy nations were able to capitalize on that early lead in securing what was, in some cases, enough to vaccinate their populations multiple times over. Canada, the US, the UK and the European Union all began Covid-19 vaccinations in December 2020. Japan started its rollout in February 2021.
But the world’s poorest economies had to wait weeks for doses to trickle in. Deliveries to poor nations through the vaccine alliance Gavi-run mechanism Covax began in February but provided limited numbers of vaccines as it too struggled to find available inoculations.
By April, Covax had split 38 million doses among more than 100 economies, the WHO announced in a statement. The UK, meanwhile, had secured roughly that amount for itself in Johnson & Johnson vaccines alone, as part of early deals for 500 million doses.
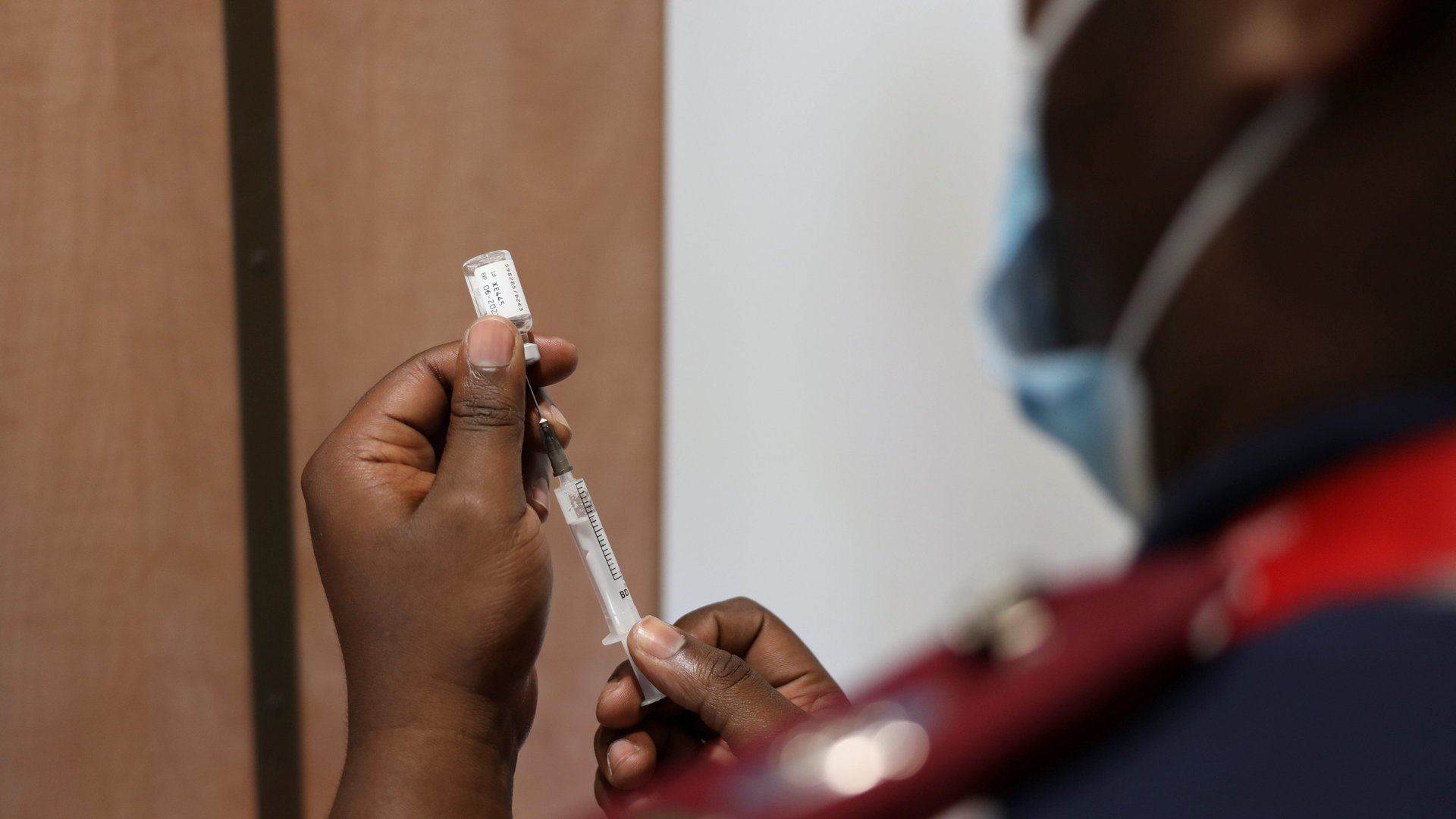
Covax managing director Aurélia Nguyen has accused pharmaceutical companies of prioritizing richer countries’ orders over fulfilling commitments to Covax. Meanwhile, many countries have not followed through on promised vaccine donations. Those that have, have done so in an ad hoc manner, with little notice, the Africa CDC, Covax, and the African Vaccine Acquisition Trust said this week, making it challenging to roll out vaccine campaigns. Supply chain disruptions are also resulting in shortages of equipment needed to deliver the vaccines, such as syringes.
South Africa’s vaccination rate
South Africa’s challenges in vaccinating its population illustrate the complexities of ensuring widespread coverage. It has had better access to Covid-19 vaccines than many other African countries through bilateral deals for jabs, and also paid to receive vaccines through Covax.
The country is racing to vaccinate 28 million people before the year’s end to reach its target of 70% coverage and, the health department says, save an estimated 20,000 lives.
While South Africans have shown high rates of vaccine acceptance in surveys, just under 40% of adults were fully immunized as of Dec. 3.
This is the result of financial and logistical challenges in accessing free vaccines, as well as vaccine hesitancy, David Harrison, CEO of the nonprofit DG Murray Trust, and leader of the government’s Covid-19 vaccine demand creation task team said in September.
“Twelve million people have applied for an R350 ($21) emergency Covid-19 relief grant,” he said. ”If you’re asking those people to pay R20 for a taxi fare to and from a vaccine site, it’s a significant trade-off.”
Data from South Africa’s early vaccine rollout suggested that people were most likely to visit a vaccination center if it was within three kilometers (1.8 miles) of their home, Harrison said: “We had to start thinking what would persuade people to go, for example, those next three kilometers to get to a site.”
The government has begun incentivizing vaccination, offering R100 ($6) and then R200 grocery vouchers to those 50 years and older to help offset the hidden costs of getting a free vaccine, such as transport fees, or a day’s missed wages.
Vaccine hesitancy has stymied efforts “Those over the age of 50 who are not vaccinated, some of them are unsure,” Harrison says. “35 to 49-year-olds have a strong religious overlay—they’re not necessarily anti-vaxxers, but they have this idea that ‘God will provide.’” The country has intensified efforts to provide basic information about vaccines to counter myths.
Meanwhile, in a country where nearly four out of 10 adults are unemployed, Harrison explains, many young South Africans see hunger and poverty as more immediate threats than covid-19
“In the younger age groups, we have to confront this reality that we have a very disaffected group of people who quite honestly say to us, ‘We’re hungry. We want jobs before jabs,’” he says. “We’re going to have to find a way to approach them that is not simply trying to keep banging the same drum about vaccination.”
The risk of new covid-19 variants
Whether the new omicron variant first identified in Botswana and South Africa arose there is not possible to say. But the continent’s inability to access its fair share of covid-19 vaccines does increase the likelihood that new variants will appear as the virus continues to spread.
Disparities in access to vaccination allow the virus to spread and mutate, the director of the Desmond Tutu HIV Centre in South Africa, Linda-Gail Bekker explained late last year in a podcast with the nonprofit organization African Alliance. “We have to shut down that transmission. If the transmission stops, the viruses’ replication will stop, mutations will stop, and new variants will not be born,” said Bekker, who has led several vaccine trials in South Africa, including studies involving the Johnson & Johnson covid-19 vaccine. “It all comes back to rolling the vaccine out as soon as possible everywhere.”
Although mortality rates were initially higher in rich countries, nearly nine in 10 fatalities could be in the global south, the Brookings Institution estimates.
“[Omicron] was inevitable,” Dr Ayoade Olatunbosun-Alakija, the co-chair of the African Union Africa Vaccine Delivery Alliance, told the BBC recently. “It’s as a result of the world’s failure to vaccinate in an equitable, urgent, and speedy manner,” she says, “And it is as a result of hoarding by high-income countries.”
Thankfully, Africa has seen increasing vaccine supplies in the past three months, Salam Gueye says.
And many Africans do want a covid-19 vaccine, according to a July study published in the journal Nature. The research found covid-19 vaccine acceptance was much higher in the low and middle-income nations under review than in the US (65%) or Russia (28%). The study included countries such as Rwanda, Burkina Faso, and Mozambique.
To help fill the gap in vaccines, the African Union has begun buying jabs on behalf of the continent and some Caribbean countries as part of the diaspora. Early next week, the AU is expected to release a plan to boost local vaccine production and, eventually, reduce Africa’s dependence on foreign nations for immunizations.
Sign up to the Quartz Africa Weekly Brief here for news and analysis on African business, tech, and innovation in your inbox.