To tackle the raging second wave, India needs faster updates to its Covid-19 treatment protocols
As Covid-19 breaks all previous records in India, the calls on social media for plasma donation have resurfaced.
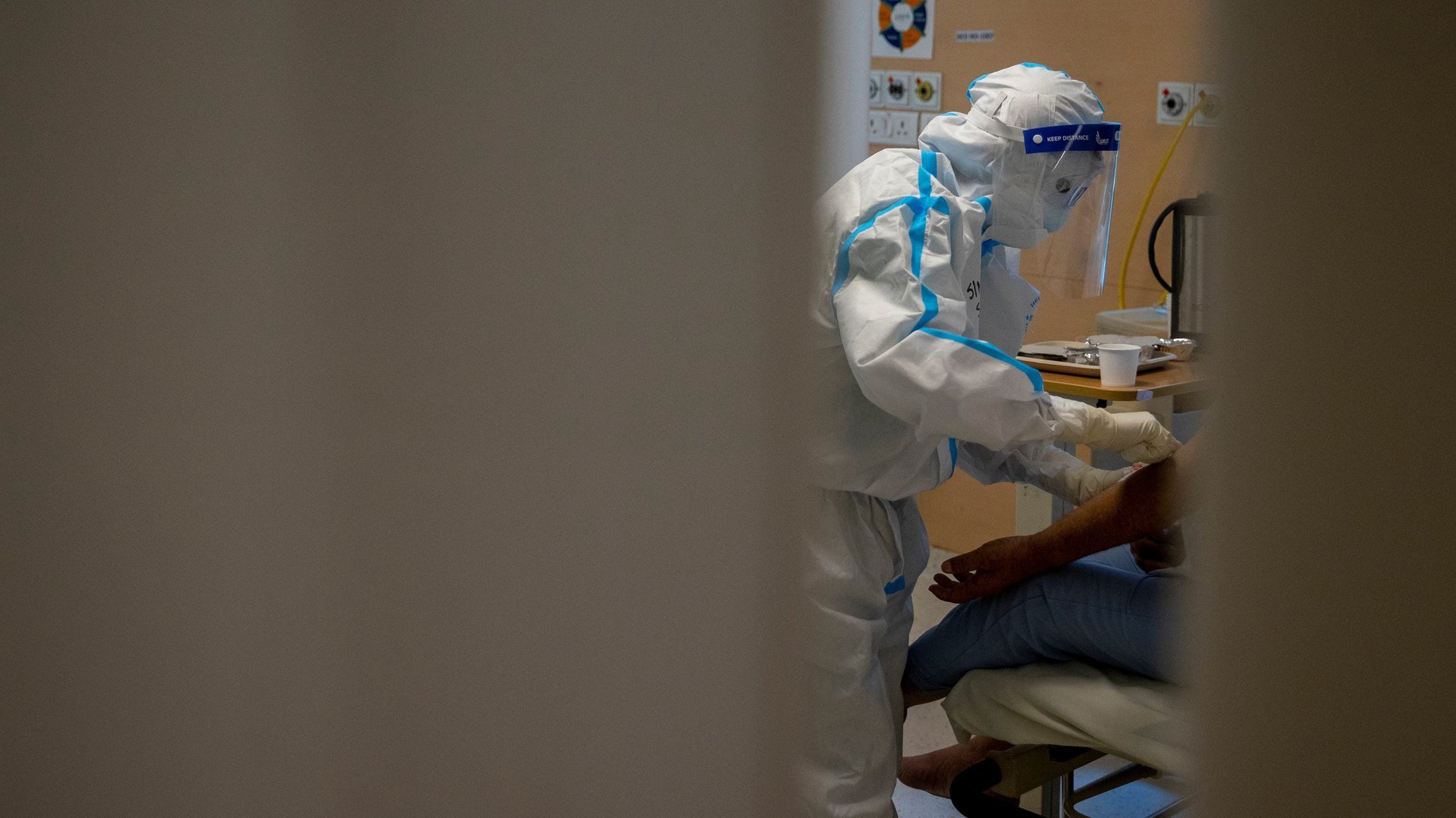

As Covid-19 breaks all previous records in India, the calls on social media for plasma donation have resurfaced.
Convalescent plasma, extracted from recovered Covid-19 patients, has been a go-to treatment option in India, particularly in cases where patients need to be hospitalised. This is transfused with the intention of preventing the infection from severe progression. Plasma therapy is also indicated to prevent the cytokine storm, a stage of the infection where the body’s immune system starts attacking itself.
Delhi’s health minister Satyendar Jain has been an advocate of plasma donation and treatment, especially since it helped during his own brush with the disease.
His and many doctors’ advocacy has remained despite various studies showing this treatment to be ineffective.
This continues to be the case for other drugs being prescribed in India under Covid-19 management protocols. Studies have found anti-malarial drugs like hydroxychloroquine (HCQ) and anti-virals like remdesivir and favipiravir to have no significant effect on mortality outcomes.
Yet, the Indian government has distributed over 100 million HCQ tablets to the states, and several Indian states are now scrambling to stock up on remdesivir injections to tackle the current surge in Covid-19 infections.
But government guidelines are slow to change, and some Indian doctors also remain divided on the effectiveness of various treatment options.
Is convalescent plasma therapy effective?
In a November study published in The New England Journal of Medicine, researchers found that “no significant differences were observed in clinical status or overall mortality between patients treated with convalescent plasma and those who received placebo.”
India’s own top medical research body, the Indian Council for Medical Research (ICMR), undertook a plasma therapy trial, one of the largest in the world, and concluded that it was ineffective in reducing mortality. Despite this trial conclusion in September 2020, the medical community remained divided on whether or not to use plasma.
For one, this has to do with a blind spot in ICMR’s own study. When the plasma trial began in April 2020, a test to check for neutralising antibodies—the kind that offers protection against the protein spikes of the novel coronavirus—was not readily available. This potentially means that there was no way to check whether those donating plasma had the right kind of antibodies to be truly effective.
Also, in most cases in India, plasma therapy is administered as a “last resort” treatment, whereas its potential benefit, if any, exists when it is administered very early in the infection curve. This theory is supported by Dr Naresh Trehan, the founder of Gurugram-based Medanta Hospital. “Given at a time when a patient is between stage two and three of the cytokine storm, the therapy can be useful. It doesn’t work when given in the late stage of the disease,” he told BBC in December.
In January, a study (pdf) published on medRxiv, a platform for pre-prints of research studies, suggested that plasma could be effective in reducing chances of serious Covid-19 disease if given to senior citizen patients within 48 hours of the onset of symptoms.
But drug treatments have fairly more conclusive evidence, some of which India continues to ignore.
HCQ, remdesivir, tocilizumab: Do they work?
In November 2020, the World Health Organization issued a recommendation against the use of remdesivir. Interim results from its Solidarity trial, which was looking at repurposing existing anti-viral drugs to manage Covid-19, found that “there is currently no evidence that remdesivir improves survival and other outcomes in these patients.”
Yet, Indian states like Madhya Pradesh have sent out urgent requests to stock up on remdesivir injections in order to provide them free-of-cost to the poor. The Indian government has asked pharmaceutical companies to prioritise remdesivir production. A British Medical Journal investigation found in December that European Union countries spent €220 million (Rs19,610 crore) stockpiling this drug despite the lack of data to prove its effectiveness.
Remdesivir can potentially have very limited benefits. Taking off from the WHO trial, a study published in The Lancet journal in November 2020 suggests that the drug is effective only when administered to those who are diagnosed with a risk of hyperinflammation, before 10 days into the infection. A US Food and Drug Administration guideline from February suggests that the use of remdesivir can reduce the recovery time in hospitalised patients (pdf).
Similarly, the window to use tocilizumab was just 24 hours after a critically ill Covid-19 patient was admitted to the ICU to improve outcomes and survival.
Even drugs like favipiravir, which some states are allegedly recommending, have been proven to be ineffective in mild cases.