Monkeypox is not a sexually transmitted infection
Two days after the World Health Organization (WHO) declared monkeypox a health emergency of international concern, the US—where official cases are close to 3,500—is considering taking similar action.
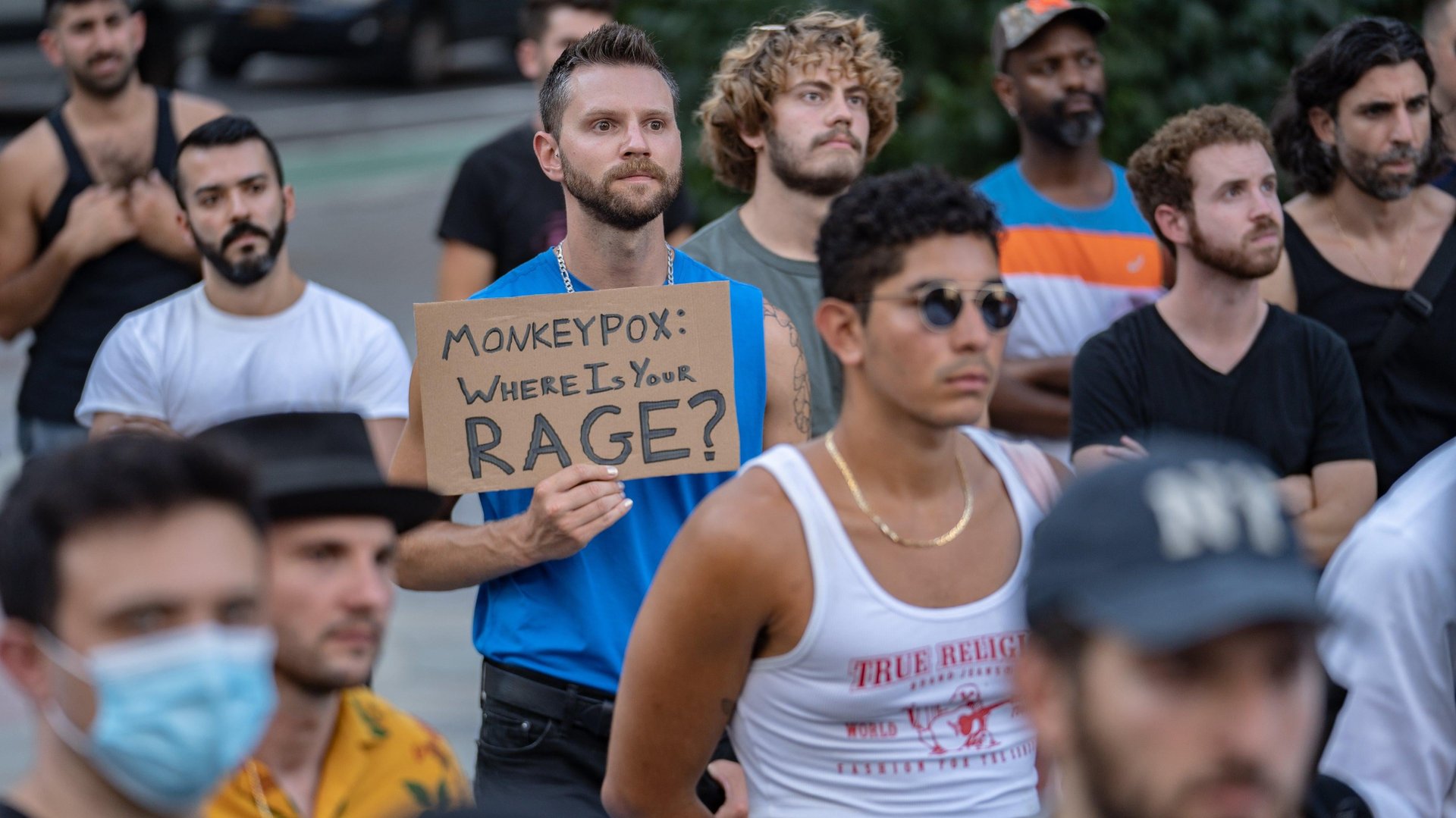
Two days after the World Health Organization (WHO) declared monkeypox a health emergency of international concern, the US—where official cases are close to 3,500—is considering taking similar action.
More than a third of the cases have been recorded in New York City, where confirmed infections have passed 1,000, and public health experts believe the documented cases might represent less than a tenth of the actual outbreak.
Globally, cases total at least 17,000, increasing by about 50% in a week. No deaths have been linked to the outbreaks in the US or Europe, but the Central African Republic and Nigeria—where monkeypox is endemic—have reported five deaths so far this year.
Most of the patients so far, in the US as well as worldwide, have been men who have sex with men, yet with delays in widespread testing and vaccines—including in the US, where there is a national stockpile—the infection is likely to become more common among other communities, too.
So far, the main focus for prevention has been on men who have sex with men, who have been offered the limited number of available vaccines—though only a small percentage have been able to get a first dose. (Despite having 100 million doses in its stockpile, the US has only made 374,000 doses available and distributed just 191,000 doses to state and city health departments, with plans to have access to 6.9 million doses in 2023).
While this focus has helped health officials share information and updates on the outbreak with the LGBTQ+ community and use sexual health clinics to distribute vaccines, there is a danger that the broader population will think of monkeypox as “a gay disease.” This, combined with the misconception that the disease is primarily a sexually transmitted infection, risks increasing stigma against men who have sex with men, as well as a false sense of security among those who fall outside that group.
Not a “gay disease”
An example of the pervasiveness of the narrative that monkeypox is a “gay disease” was provided on Friday, when two children tested positive. Discussing the cases, Rochelle Walensky, the director of the Centers for Disease Control and Prevention (CDC), noted that “both of those children are traced back to individuals who come from the men-who-have-sex-with-men community, the gay men’s community.” The way this is phrased though, omits the most important element: That the contagion happened via household transmission, something that has nothing to do with the sexual habits of the people living in the home. The news came a week after Dutch researchers announced that a child in the Netherlands had contracted monkeypox with no known source for the infection.
The focus on the sexual component of monkeypox transmission is entirely unjustified. Last week, the Associated Press reported that some experts fear that monkeypox “is becoming so widespread that it is on the verge of becoming an entrenched STD—like gonorrhea, herpes and HIV.” This is incorrect: monkeypox is not a sexually transmitted disease (STD) or infection (STI). In fact, WHO researchers aren’t even sure that it can be transmitted through semen or vaginal fluids, though some preliminary results of recent studies suggest so.
Misinformation is making it more difficult to inform the public about the disease as inaccuracies about monkeypox transmission get mixed with conspiracy theories about the virus, new research from MIT Technology Review by the Center for Countering Digital Hate has shown.
Scientists are now beginning to test for monkeypox in wastewater as a way to get true estimates of the spread. Currently, only patients with lesions can get a monkeypox test and it takes up to two weeks for those boils to appear.
How monkeypox is transmitted
Monkeypox’s main avenue of transmission is through skin to skin contact with an infected person, as well as with fabrics, such as bedsheets, towels, and clothing, that have been in close contact with the ill person for a prolonged period of time. Respiratory secretions (large droplets resulting from sneezing, for instance, as opposite to the small aerosols that spread covid) can also spread the virus, as can fetal contact with the placenta of a symptomatic mother.
It is yet unclear, but seems unlikely, that the virus can live on and spread through other surfaces, such as door knobs, or subway poles. It is also under investigation whether asymptomatic transmission occurs, but so far it appears that only people who have developed symptoms—ranging from flu-like ones to the more characteristic rashes and sores—are contagious.
Of course, sexual interactions typically involve skin to skin contact, so having sex with someone who is symptomatic is a risk for infection, but nonsexual contact, or even sharing linens and household items, can lead to illness, too. So while sex can lead to transmission, it is not the primary mode, and people need to stay vigilant to other avenues of transmission.
This is important to understand as outbreaks continue to grow, so that people adopt the correct precautions, in particular by paying attention to any rashes or sores and avoiding contact with others if they emerge.