Study: Viable pregnancies may be getting misdiagnosed as miscarriages
Doctors and hospitals need to adopt extra steps to make sure they aren’t mistakenly telling pregnant women that they’re going to miscarry, say the experts of a large new study.
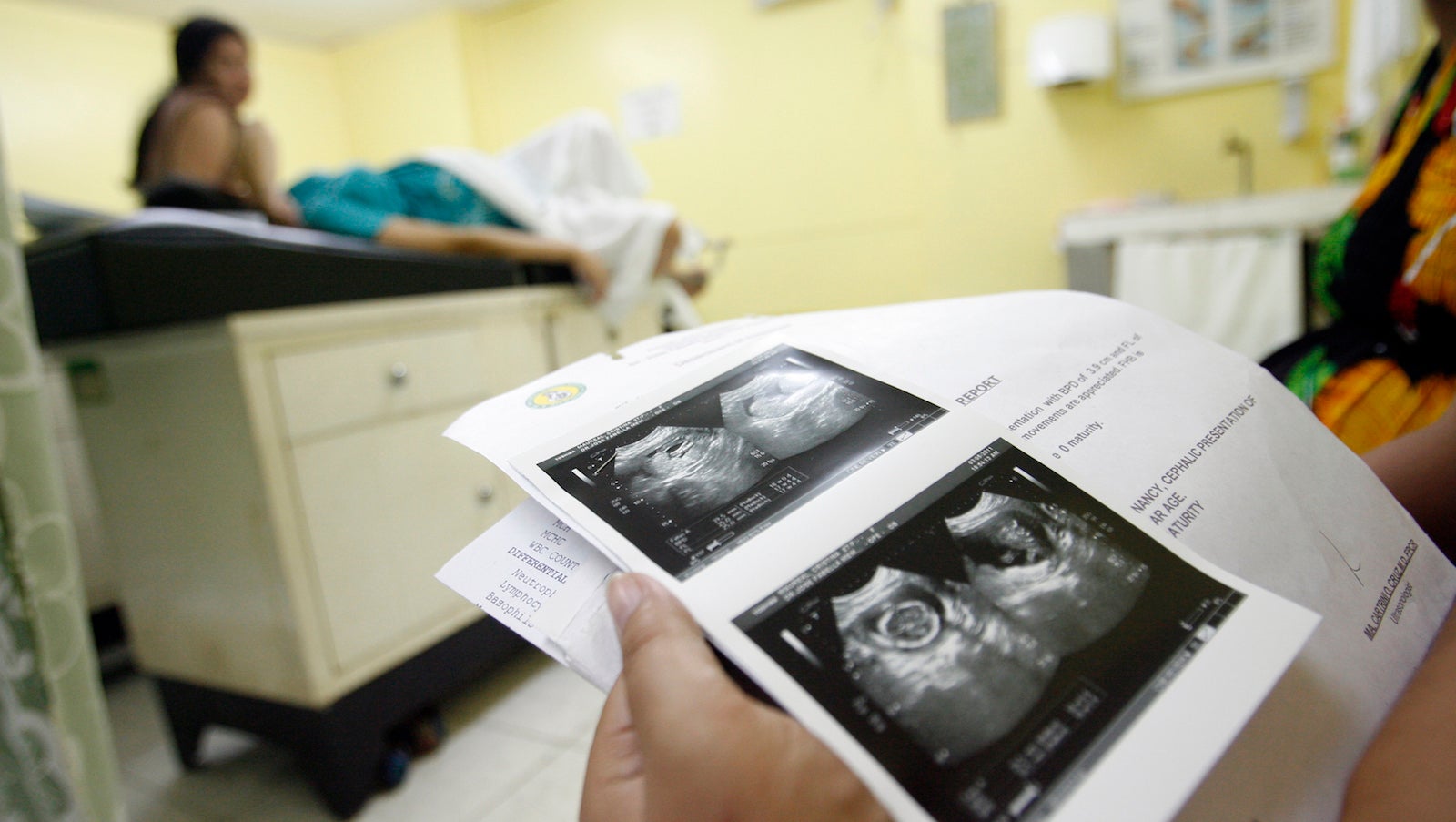

Doctors and hospitals need to adopt extra steps to make sure they aren’t mistakenly telling pregnant women that they’re going to miscarry, say the experts of a large new study.
The study—produced by a team of medical experts and professors from hospitals and universities in the UK and Belgium—was published this week in BMJ Open Journal. It studied around 3,000 pregnant women in Britain whose doctors believed they might have a chance of miscarrying because they were bleeding or experiencing pain. Out of 549 initial miscarriage diagnoses, 19 were wrong: New ultrasound scans two weeks later showed that these pregnancies were viable after all.
Miscarriages are predicted by doctors when a woman’s embryo or gestational sac seems too small, and when an ultrasound shows no fetal heartbeat. (In the cases included in the study, doctors had detected a gestational sac in the uterus, ruling out the risk of an ectopic pregnancy.) After receiving this diagnosis, a woman can either have surgery, wait for the miscarriage to happen, or take medication to trigger it.
But according to the researchers, it’s not always true that a small embryo without a detectable heartbeat is going to be a miscarriage—so doctors should always follow up with their patients for a second ultrasound in two weeks.
The study builds on previous research in 2011 that showed some old hospital guidelines for diagnosing miscarriage based on the size of the embryo or gestational sac in Britain were too rigid. Many British health services then announced new standards that a second scan should be offered. Based on this recommendation, some doctors informally adopted 7 days as a rule of thumb for the wait period on conducting the second scan. But the official guidelines should stipulate a 14-day wait and provide more detail about the range of viable embryo sizes relative to how far along the woman is, the study’s researchers say.
“We are talking about a small number of cases, but remember there should be no errors over something as important as this,” Tom Bourne, a gynecologist and the study’s lead author, told The Guardian. “Women should be able to rely on a diagnosis of miscarriage. It’s an area of medicine where the highest levels of caution are warranted.”
Two Australian medical experts added an editorial to the study, writing: “The diagnosis of a miscarriage will more than likely dash the hopes and dreams of couples anticipating the life changing possibilities of a new addition to their family—a new house, extended leave from work, relief in finally appeasing grandparents-in-waiting. It is therefore paramount that clinicians get it right. Always.”