What an unsupportive work environment actually costs nursing mothers
World Health Organization guidelines suggest babies should be exclusively fed breastmilk up to the age of six months, and that infants are healthiest when breastfeeding continues, alongside other feeding, up to at least the age of two years. For women with full-time jobs, it’s a huge challenge—especially in places like America, where paid family leave isn’t mandated and maternity leaves are comparatively short.

World Health Organization guidelines suggest babies should be exclusively fed breastmilk up to the age of six months, and that infants are healthiest when breastfeeding continues, alongside other feeding, up to at least the age of two years. For women with full-time jobs, it’s a huge challenge—especially in places like America, where paid family leave isn’t mandated and maternity leaves are comparatively short.
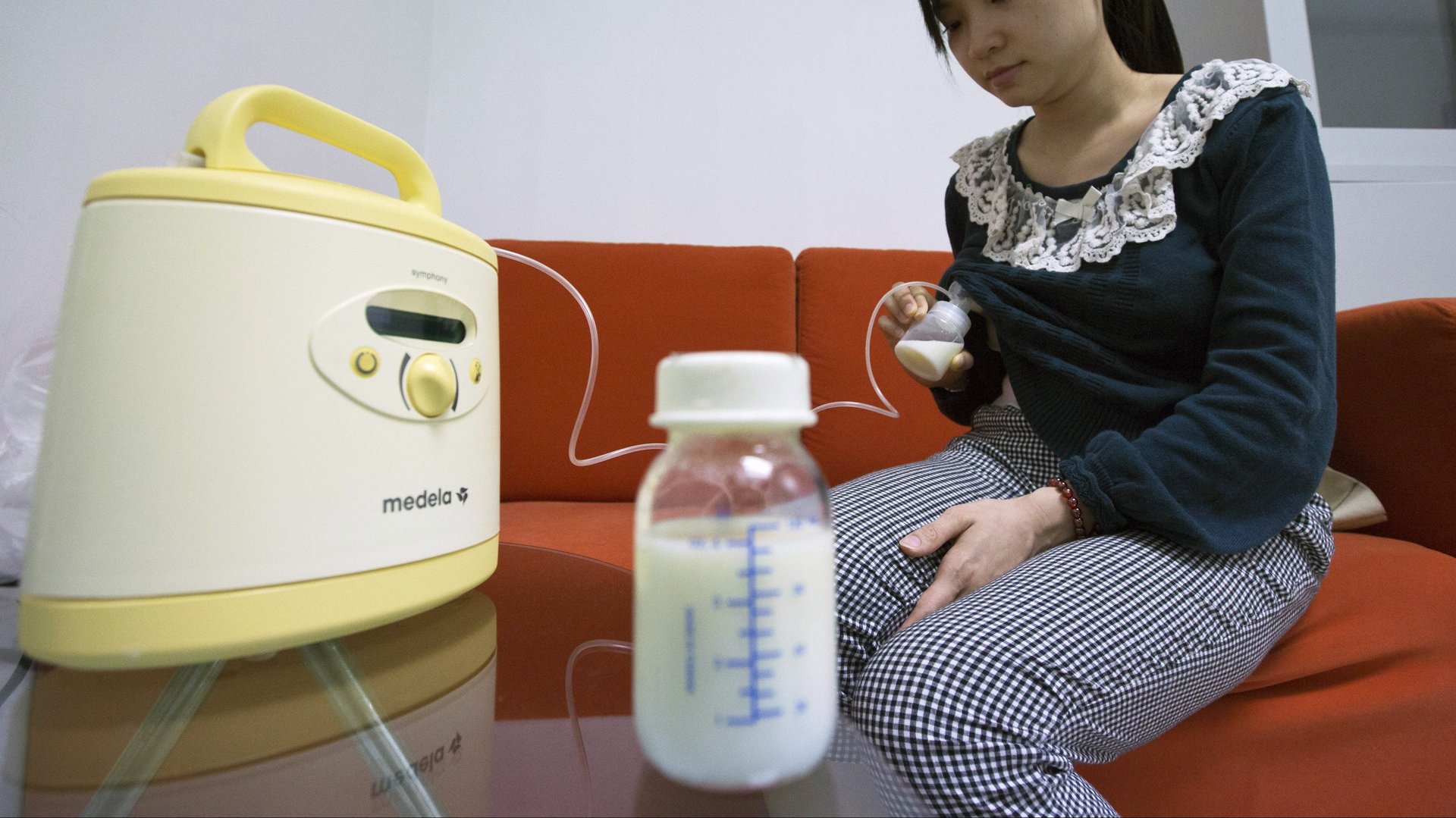
Returning to the office within months or even weeks of giving birth means that nursing mothers who want to continue feeding their babies breastmilk often have only one option: regularly pumping every three to four hours (that’s how frequently babies tend to feed, so that’s the schedule breastmilk production adheres to), for as long as it takes to extract the required amount—typically 15 to 30 minutes per session.
And that’s just the start of the work to be done to make pumping successful: Pumps and bottles need to be sterilized beforehand and cleaned after, breastmilk must be refrigerated, and a designated space must be located to do the pumping. If there isn’t one available, women will have to improvise: pumping in private offices, bathrooms, and even cupboards is by no means unusual.
A new study shows that all these conditions have a material effect, and not just on women’s wellbeing. According to the research, women who aren’t supported to pump at work find themselves less able to complete their work tasks—and they produce less milk than happier, better-supported nursing mothers in the workplace.
The research comes from the University of Arizona and is published in the Academy of Management Journal. For their first study, researchers interviewed 38 women who worked full-time and pumped at work. In a second study, they surveyed 106 women who were working full-time and breastfeeding or pumping at least three times a day, following them for 15 days.
Women who reported more difficulties in the experience of pumping at work also self-reported as being less focused on work goals later in the day. And compared to women who reported happier experiences, they didn’t produce as much milk. The researchers found “a significant relationship between experiencing a sense of enrichment (i.e., feelings of accomplishment, success, and fulfillment) and the ounces of milk produced that day,” one of the study’s authors, Marcus Butts of Southern Methodist University in Texas, explained in an email. Specifically, for every “unit” of increased feelings of “enrichment,” women produced 1.12 oz more milk than the average (12.27 oz compared to an average of 11.25 oz).
What conditions made women feel that the experience of pumping at work was “enriching,” or the opposite? Interviewees talked about problems of scheduling—finding time to pump within busy work schedules—and restrictions on space, including an internal office “commute” from their desk to a designated pumping space. One participant reported a walk of 15 minutes each way to the nearest pumping room, while another reported days of back-to-back meetings without time to pump in between.
The good news, said Allison Gabriel, the study’s lead author and an associate professor at the University of Arizona’s Eller College of Management, is that when women reported breastfeeding going well at work, the success “correlated with lower negative emotion, which in turn resulted in higher self-reports of work productivity and breastmilk [production].”
It should be noted that not all babies have mothers, not all women can breastfeed, and some don’t want to. But for those who do, support in the workplace is vital. Other research has found that colleagues are even more influential than family and friends when it comes to encouraging nursing mothers to continue pumping at work.