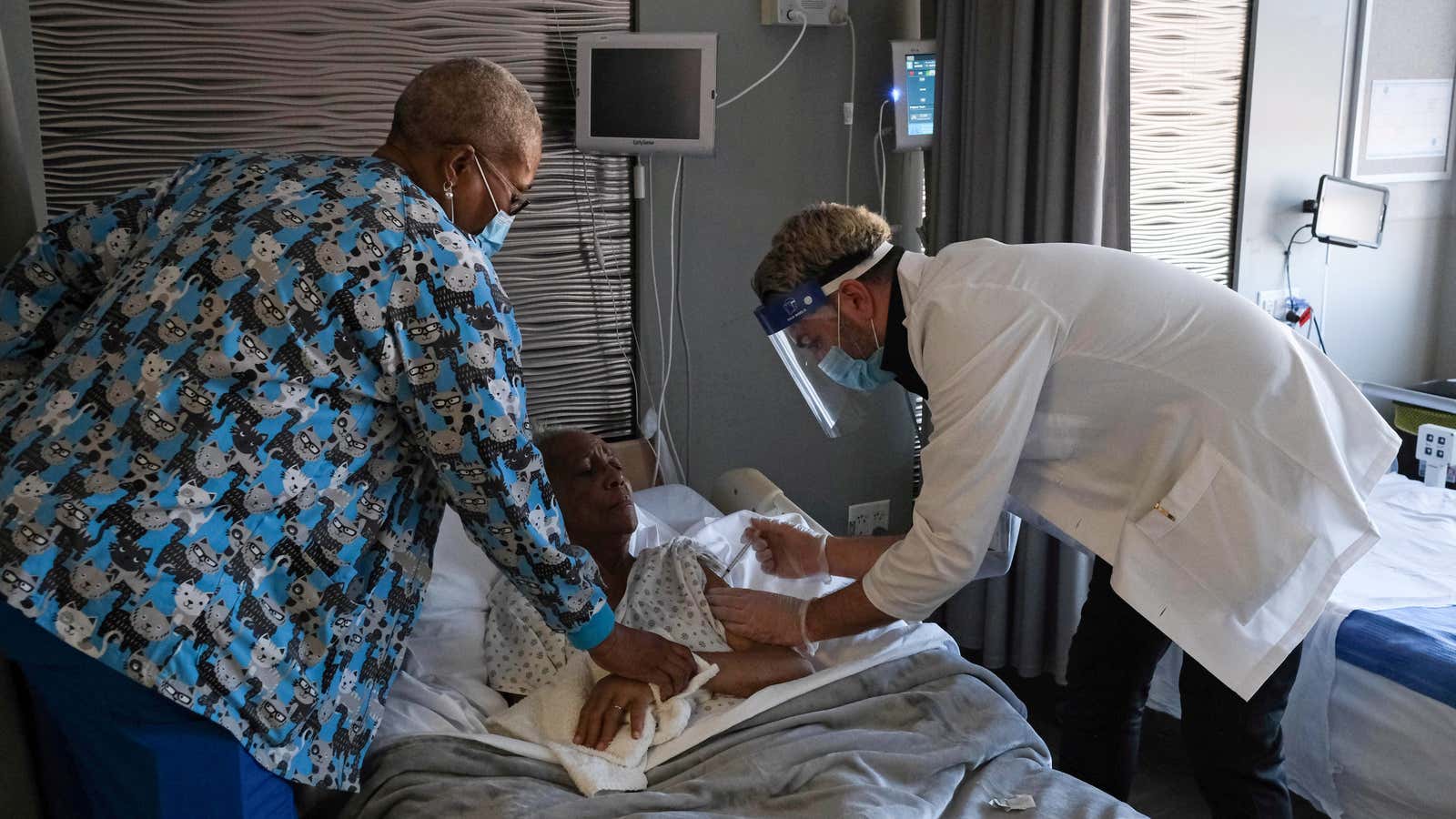
Of the roughly one million Americans who have died from covid about 150,000 have been nursing home residents. One million US nursing home workers have also been infected by the virus and more than 2,000 have died because of it.
But not all nursing homes suffered losses at the same devastating scale, and researchers are working to untangle the myriad reasons why. A new study adds an important piece to the puzzle: It finds that unionized nursing homes were safer places to be during the height of the pandemic.
The study looked at data from more than 13,000 US nursing homes—that is, nearly every facility in the 48 continental states—and found that overall, covid death rates in nursing homes with a unionized workforce were 10.8% lower than death rates in nursing homes with a non-unionized workforce. Unionized staff were also 6.8% less likely to be infected compared with their non-unionized counterparts during that period.
By extrapolation, had all US nursing homes been unionized during the one year studied (beginning in June 2020), some 8,000 resident lives could have been spared, the authors report.
“Unions were fighting to protect nursing home workers,” Adam Dean, professor of labor politics at George Washington University, tells Quartz, “and in doing so, they not only lowered worker infection rates, but also had these broader benefits for society, namely, reducing resident mortality rates.”
How unions might make nursing homes safer
Previous research comparing unionized and non-unionized healthcare settings has also found a link between unionized labor and better health outcomes. Like those studies, this one doesn’t prove that unions cause more positive results. However, the study outlines several reasons why that might be the case.
For one thing, unions made heroic efforts to keep their members from getting sick at work, says Dean. “We know that unions have been fighting for access to personal protective equipment for workers. We also know that unions have been fighting for paid sick days.” Both sick pay and access to equipment like masks, gowns, and gloves, have been connected to safer workplaces, he adds.
“It’s pretty simple,” Rosalind Reggans, a certified nursing assistant in Illinois told the investigators. “The safer we are, the safer they are.”
Unionized employees may have also been more likely to speak up against hazardous practices, or to insist on isolating residents that tested positive, without fearing for their jobs or suffering other forms of retribution, the authors argue. Their collective action may not be as visible as the unionization drives and protests we’re seeing at big brand name companies like Amazon, Starbucks, and Apple, says Dean, but union campaigns at nursing homes “don’t always take the form of strikes.”
“Workers often have fine-grained knowledge of what’s going on within nursing homes and need a mechanism with which to share those concerns with management,” he explains. Unions provide that line of communication. He and his researchers heard several stories about unionized employees taking their concerns about infection control policies to union leaders so that their representatives could speak directly to nursing home management about making changes to limit staff and resident exposures.
Long-term care staff whose unions ensure good pay and benefits tend not to work in more than one facility, he adds. Other non-unionized senior care workers commonly have little choice but to take on a second job, which has been one way covid-19 has jumped between homes during the pandemic: asymptomatic workers have unknowingly carried it between their workplaces.
The researchers’ findings—which build on a smaller study about New York state nursing homes—took into account several other factors that may explain higher survival rates at some institutions, such as better staff to resident ratios.
Nursing home workers have long deserved pay increases and better jobs
Experts have decried the low pay and demanding working conditions facing senior care nurses and staff for decades. Skilled nursing homes have not received adequate federal funding, say industry critics, while profit-seeking private equity and real estate trust groups have sought to keep costs—including labor costs—down.
During the pandemic, both unionization drives and strikes among unionized nursing home workers increased dramatically, NPR reports. “The urgency and desperation we’ve heard from workers is at a pitch I haven’t experienced before in 20 years of this work,” Cass Gualvez, organizing director for Service Employees International Union-United Healthcare Workers West in California, said last year.
“We’ve talked to workers who said, ‘I was dead set against a union five years ago, but covid has changed that,'” he added.
Still, the drives were not always successful. And the rise of organized labor within the field has not stopped hundreds of thousands of employees from quitting during the pandemic. Speaking to the Washington Post recently, David Grabowski, who studies the economics of aging and long-term care at Harvard Medical School called the labor crunch situation in senior care “a crisis on steroids,” adding that the “long-standing issue of underinvesting and undervaluing this workforce is coming back to bite us.”
Unionization, already common at homes in northeastern states, could make the profession more attractive, says Dean. He and his team found that staff at only 17% of US nursing homes were protected by organized labor agreements, but he’s optimistic that more nursing home employees will unionize, especially knowing that it could make a life-saving difference.
“A lot of what our work is trying to do is to remind people that these [improved] workplace conditions aren’t just free floating or randomly determined,” he says, “unions played an active role in fighting for those conditions.”