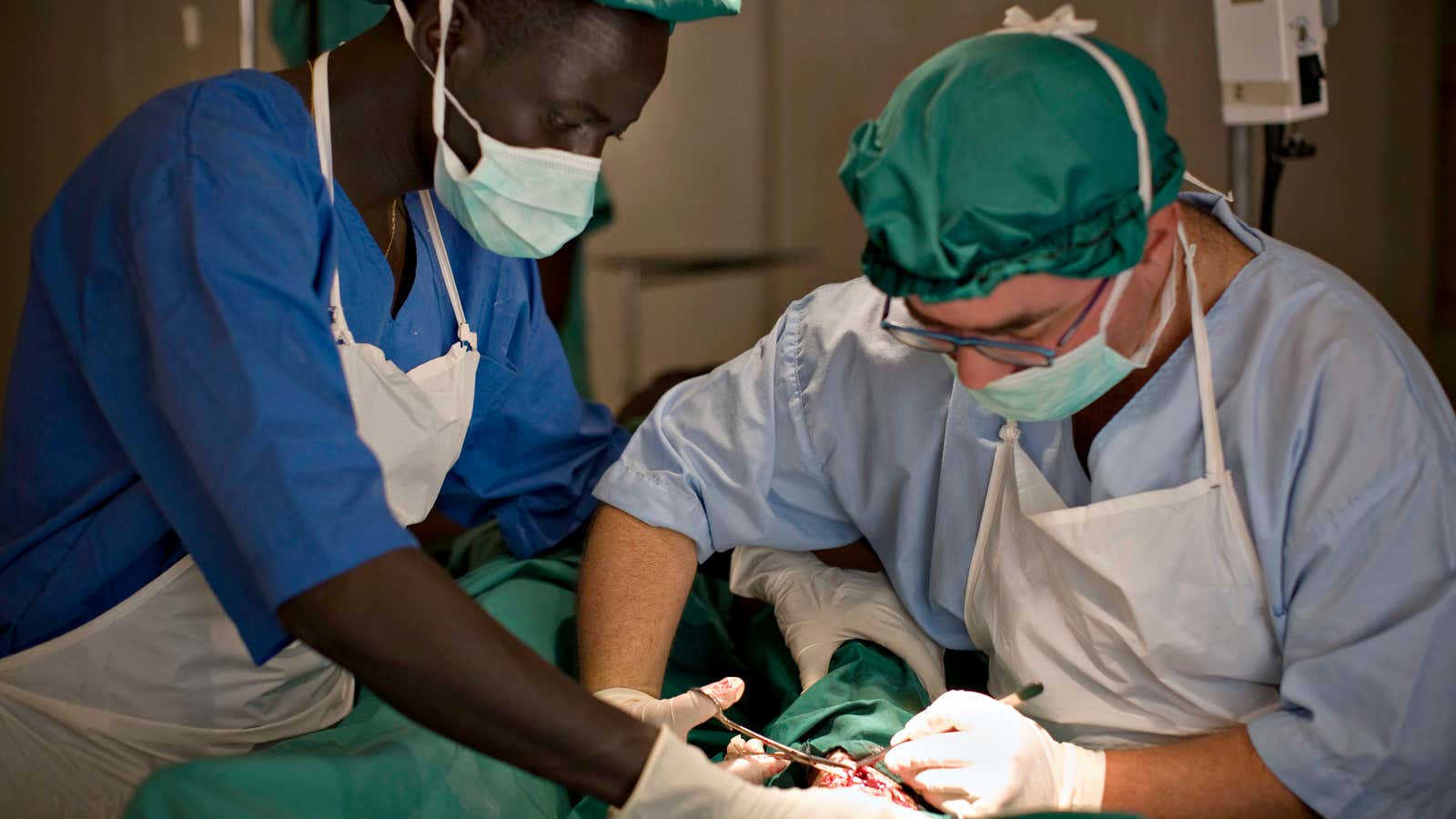
One hot, December day, a twenty-one year old man who appeared healthy arrived at Tygerberg Hospital here in Cape Town and some time later was ushered into theatre. He remained there for nine hours.
The young man was there because just three years earlier he had had his penis amputated in order to save his life after a local circumcision had gone badly wrong.
The surgery he underwent in December was declared a success just four months later: he was the recipient of the first-ever penile transplant to result in full functionality.
Though he has asked to remain anonymous for privacy reasons, his medical team has, understandably, been very publicly jubilant.
“We are fortunate, and very, very thankful, that things went well,” said neurologist Andre Van Der Merwe, who led the surgery.
“I think people are pessimistic – understandably so – about aspects of South Africa. What I am glad of is that we can at least show that we can still do something that nobody else done, with the resources that we have.”
While the global perception of Africa’s healthcare standards is dominated by images of Ebola, HIV/AIDS and other contagious diseases, it is not the first time that doctors in the continent’s most advanced economy have broken ground. South Africa surgeons pioneered the heart transplant in 1967.
Elsewhere in the world a penis transplant might seem somewhat outlandish or even a vanity project. But in South Africa, the success has an important significance driven by unfortunate circumstances. Professor Van Der Merwe’s patient was one of scores of victims of botched traditional circumcision ceremonies every year.
Arguably, he was one of the luckier ones.
Dangerous Initiation
Every year, reports of a new wave of avoidable deaths invariably follow initiation season. Twice a year, at the height of summer and winter, tens of thousands of young men of the Xhosa people venture into the bush to complete the ‘journey to manhood’. The ancient rite of passage is three weeks long: a physical and psychological endurance test that is essential to a man’s standing in society.
During this time, ‘traditional surgeons’ – most of whom do not have formal medical training – perform the circumcision ceremonies. Blade is brought to skin without anesthesia, and often in unsterile conditions. Some of the boys are lucky, escaping infection or recovering from it. But while each boy waiting his turn hopes that he will fall into that fortunate group, nearby hospitals prepare for an influx of youngsters who return with septicaemia, gangrene, severe dehydration and other illnesses. Each year, an estimated 200- 250 young boys are hospitalized in the Eastern Cape alone, according to Van Der Merwe. In 2013, 33 deaths were recorded in that province in the space of just two weeks.
Compounding the dangers of infection are ‘bogus traditional healers’ looking to piggyback off a profitable practice, and the reluctance of injured boys to seek medical help.
“It is traditionally seen as a severe weakness to seek any form of help from Western hospitals,” says Van Der Merwe. “So what we are seeing is just the tip of the iceberg.”
Bad Practice
Although the practice has come under severe criticism from health authorities and groups, the South African government has resisted banning initiation schools, which are regarded as sacred by many communities. Efforts have been made however, to provide training to traditional surgeons on surgeons, encouraging partnerships between local clinics and initiation schools.
Thus far, however, efforts to increase the acceptability of medical circumcision – also important as an HIV prevention measure – have met with limited success. While slowly, perceptions may begin to change in light of the costs of protecting tradition, for many, the process is too lengthy.
Until unsafe practices are entirely eliminated, botched circumcisions will keep happening. And demand for the procedure that Professor Van Der Merwe and his team pioneered will, sadly, continue to grow.