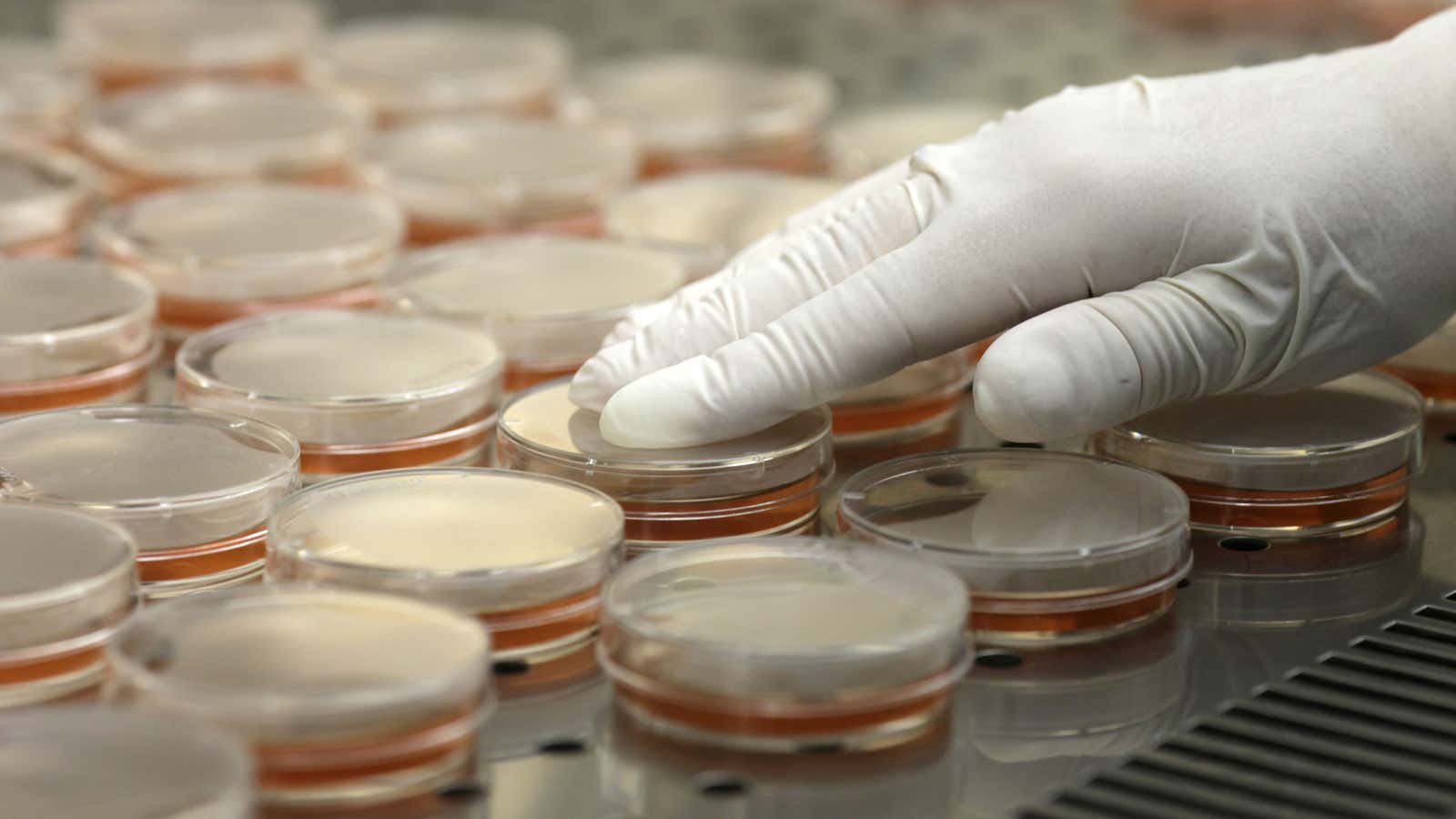
Ah, science: The objective roadmap for solving life’s most pressing questions. And also, for figuring out whether or not human farts emit harmful bacteria.
Sixteen years ago, a nurse asked Australian physician Karl Kruszelnicki if her flatulence could contaminate a sterile operating room. Her concern was that the patient on the table would be at risk of developing an infection as a result of her gas.
So Kruszelnicki asked a colleague to fart into a small petri dish used for growing bacteria once with pants on, and once in the buff. He found that on the petri dish exposed to the naked fart, colonies of common gut and skin bacteria began to grow overnight.
His glorious conclusion, published in a short blurb in the British Medical Journal, reads as follows:
“Our deduction is that the enteric zone in the second petri dish was caused by the flatus itself, and the splatter ring around that was caused by the sheer velocity of the fart, which blew skin bacteria from the cheeks and blasted it onto the dish. It seems, therefore, that flatus can cause infection if the emitter is naked, but not if he or she is clothed. But the results of the experiment should not be considered alarming, because neither type of bacterium is harmful. In fact, they’re similar to the ‘friendly’ bacteria found in yoghurt.”
So, patients are not actually at risk if their surgeons fart. Which is lucky, because in 16-hour operations, doctors will inevitably have to let some wind loose.
Flatulence research is hardly limited to this one experiment. Scientists have been studying our gas for years as a way of understanding digestive disorders.
They’ve learned a lot along the way: As FiveThirtyEight points out, an average fart emits roughly enough gas to fill a bottle of nail polish or a can of soda. These farts are made up mostly of hydrogen and methane, which come from bacteria in the colon feasting on the parts of our meals we aren’t able to digest ourselves—like lactose in milk, or complex carbohydrates found in beans and legumes.
Not all farts are created equal. Everybody breaks down food differently, as do their unique bacteria. “A gas smell is as characteristic of a person as a fingerprint,” Alan Kligerman, CEO of AkPharma, the company that developed the anti-gas pill Beano, told Mary Roach in her book Gulp.
Roach also describes the work of Michael Levitt, a physician in the Department of Veterans Affairs in Minnesota, who spent a large part of his career studying these smells to figure out what causes them. Levitt actually employed a team of fart judges to rank smells from “no odor” to “very offensive.” His team found that hydrogen sulfide is reminiscent of rotten eggs, dimethyl sulfide is more sweet, and methanethiol reeks of rotting veggies. This work has led to a diagnostic tool for diseases characterized by the inability to absorb nutrients in the small intestine, which can be life-threatening if untreated.
We can all agree that everybody farts—and that, if you’re a doctor or nurse, you should probably keep your pants on in the operating room. “It’s not rocket science,” Kruszelnicki said. “But then again, maybe it is?”