Apple is reportedly working on a “super secret” medical project: building sensors to monitor blood sugar levels without piercing the skin.
According to CNBC, the iPhone maker has been working on this for at least five years, quietly hiring dozens of biomedical engineers and sequestering them in a nondescript Palo Alto office.
It may be intended to connect to the Apple Watch, which Apple CEO Tim Cook has previously hinted at trying to make more medically useful, even suggesting that an app developed “adjacent to it” might have to get approval from the US Food and Drug Administration. And Reuters reported in 2014 that Apple, Samsung, and Google were all interested in merging their respective mobile devices with glucose monitoring devices. What Apple’s reportedly trying to do here hasn’t worked out so well for Google, whose life-sciences arm, Verily, is also located away from company headquarters in its own unassuming office building and has long been working (publicly) on a smart contact lens for blood sugar monitoring. That project hasn’t been fruitful yet.
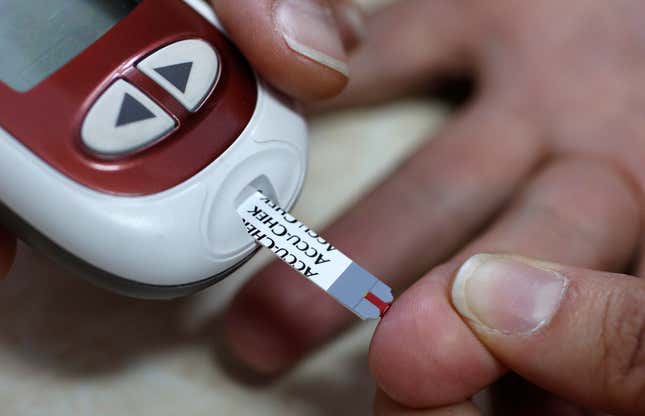
Keeping track of how blood sugar levels rise and fall throughout the day is a big job for people with type 1 diabetes, whose bodies don’t produce insulin—a crucial hormone in blood sugar regulation. Diabetics typically test blood samples from their fingertips several times a day to measure these levels, but since the numbers can fluctuate so much in response to food, exercise, stress, and other factors, a few data points per day isn’t always enough information. That’s why enthusiasm has been building for continuous glucose monitoring (CGM) sensors.
These sensors rely on a small needle that stays under the skin for days at a time to analyze interstitial fluid—the stuff that surrounds tissue cells—to measure blood sugar and wirelessly transmits the data to a receiver with a screen displaying the numbers. Dexcom, the current leader in CGM, has a sensor that works with an app for the iPhone and the Apple Watch.
According to CNBC’s report, it sounds like whatever Apple’s working on would only differ by using light or an electrical current instead of a needle under the skin. Dexcom’s technology is considered “minimally invasive,” while an optical or electrical sensor would be “non-invasive.”
This has been tried, unsuccessfully, in the past. Most notable, perhaps, was the commercial failure of a device called the GlucoWatch, which was approved by the FDA in 2001. It was worn just like a regular wristwatch and sent electrical currents through a patient’s skin to test blood sugar levels every 20 minutes, displaying the numbers on its face so that checking a blood sugar was as easy as checking the time. It was described in FDA documents (PDF) as ”a device that provides frequent, automatic, non-invasive glucose measurements. The glucose sample is obtained directly through intact skin.” It may have met the definition of non-invasive, and it may have been accurate, but it was also painful.
“It generated an electrical current, and for many people it caused a burn,” according to Henry Anhalt, an endocrinologist who had patients that tried the device. Anhalt, now the chief medical officer at a diabetes research network called the T1D Exchange, says that although the GlucoWatch provided accurate results, “people felt this burning sensation which I believe led to the demise of the product. Collectively in the community we were all discussing that this was why patients stopped using it.”
Since the early 2000s, companies like Dexcom, Abbott, and Medtronic have successfully brought minimally invasive CGM devices to market, though Dexcom ran in the red for years, Abbott shut down its diabetes division in 2011, and Medtronic’s sensors were hampered by quality control problems for several years. Today, Dexcom is profitable and several hundred thousand people in the US use either its CGM or Medtronic’s. Some people with diabetes consider them “must-haves,” but not all. And it’s not clear that a sensor made by Apple, despite being non-invasive and from a trusted consumer brand, would be a “must have,” either.
“These devices haven’t crossed the return on investment yet for a lot of people,” Aaron Kowalski, one of the research leads at the Juvenile Diabetes Research Foundation, recently told Quartz. Glucose sensors will become bigger game-changers once they’re hooked up to automated insulin delivery, or “closed-loop,” systems, like the soon-to-launch Medtronic insulin pump, which has an integrated CGM that triggers the pump to suspend insulin delivery when low blood sugar is detected. Future devices are supposed to be capable of even more, and the true “holy grail” for many diabetics, short of a biological cure, is a fully-closed loop system that doesn’t require them to even look at or think about their blood sugar numbers—hopefully because a computer is constantly making its own decisions based on those numbers.
