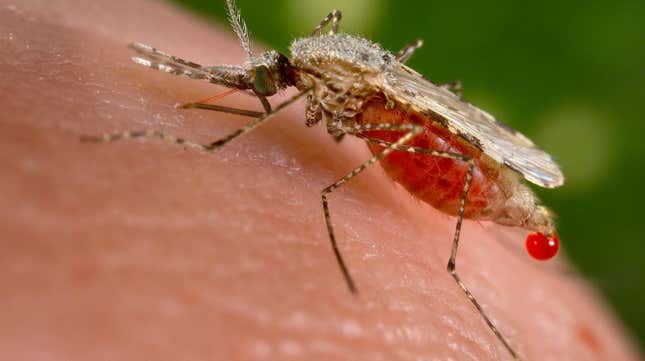
The biggest hurdle in eradicating malaria is that the parasite is highly adaptable and resistant, and nascent vaccines are only partially effective. Genetically-engineered bacteria have long been touted as potential malaria-enders but they’re complex to develop. Researchers now think they have found a more straightforward way to end the spread of the disease: naturally occurring bacteria that stops the development of the malaria parasite in the insects’ guts.
Scientists at a GlaxoSmithKline (GSK) research facility in Spain discovered that a strain of Delftia tsuruhatensis bacterium, named Tres Cantos 1 (TC1), inhibits the malaria parasite in mosquitoes, known as Plasmodium. Researchers suspected something was going on when the mosquitoes they were using to study malaria were resisting Plasmodium infections. As noted in the study published in the peer-reviewed journal Science yesterday (Aug. 3), TC1 secretes a molecule called harmane that attacks the Plasmodium parasite, which is transmitted to humans by the bite of a mosquito.
When the researchers fed the existing strain to other malaria-spreading Anopholes mosquitoes—without any human tinkering like with the genetically-modified microbes—they found the bacteria “drastically reduces malaria parasite burden in the mosquito, potentially reducing transmission to humans significantly,” GSK said in an Aug. 3 press release.
TC1 has another characteristic that makes it promising for regulatory approval, as it does not spread from mosquito to mosquito, therefore allowing researcher to monitor its efficacy and safety before deploying it more widely. “When you are ready to deploy in massive amounts, you would like [the bacterium] to spread. But before you do that, you really want one that doesn’t spread too much,” Carolina Barillas-Mury, who leads the malaria and vector research lab at the US National Institutes of Health and who did not work on the study, told the Science journal.
Potential malaria prevention, by the digits
619,000: Worldwide deaths caused by malaria in 2021
Every minute: How often malaria kills a child around the world, according to charity Malaria No More’s Gareth Jenkins. “With a strong innovation pipeline, it is possible to end the threat of malaria in our lifetimes,” he told the BBC
75%: Fewer Plasmodium oocysts—egglike structures the parasite forms in the insect gut–that were present in mosquitoes with D. tsuruhatensis versus the insects lacking the bacterium, according to findings from John Hopkins’ Jacobs-Lorena’s lab research
One-third: Share of mice bitten by bacterium-carrying mosquitoes that became infected, compared with 100% of mice bitten by regular mosquitoes
More than 16 days: How long the inhibition lasts for once the bacterium stably populates the mosquito midgut—typically longer than a mosquito’s lifespan
Mosquitoes or malaria parasites are less likely to develop resistance to TC1
💪 TC1 does not impact the fitness or reproductive ability of the mosquito, avoiding the natural selection of resistant mosquitoes.
🎯 By targeting the parasite in the mosquito instead of in humans, parasite numbers are much smaller. As a result, “the chances of the parasite developing resistance are greatly reduced,” GSK noted.
Quotable: A dwindling rate
“The infection rate in the mosquitoes started dwindling and so by the end of the year the mosquitoes just would not be infected with the malaria parasite.” —Janneth Rodrigues, who led the study and is named as co-inventor on a patent related to the discovery, quoted by the BBC.
Place of interest: Burkina Faso
Researchers have conducted field studies in a contained facility in Burkina Faso dubbed the MosquitoSphere, which is a roughly 10-meter-by-10-meter-by-5-meter netted enclosure designed to simulate the real world with plants and breeding areas. The scientists left out enough balls of cotton wool soaked in sugar and D. tsuruhatensis to colonize three-quarters of the mosquito population with the bacterium overnight. Like in the lab, the bacterium blocked the parasite’s development when the mosquitoes fed on blood from people with malaria. More such trials are underway in the West African nation.
GSK lead researcher Rodrigues says an eventual product could take the form of a bacterium-containing powder or even harmane itself, mixed with sugary baits to attract the insects, according to Science. But before going to market, there’s still rigorous testing to be done.
Plus, the researchers are also testing to ensure the bacterium doesn’t harm other insects such as bees before developing a product to sprinkle and spread in the real world.
Related stories
🌍 The countries with the worst malaria rates
🇬🇭 Ghana is the world’s first country to approve Oxford’s new malaria vaccine
🇳🇬 The country with the highest rate of malaria deaths in the world has approved Oxford’s vaccine