The insulin copay cap was a bad idea anyway
The Inflation Reduction Act limits the copay cap for insulin only to Medicare patients. But even as originally intended, the cap was not helpful
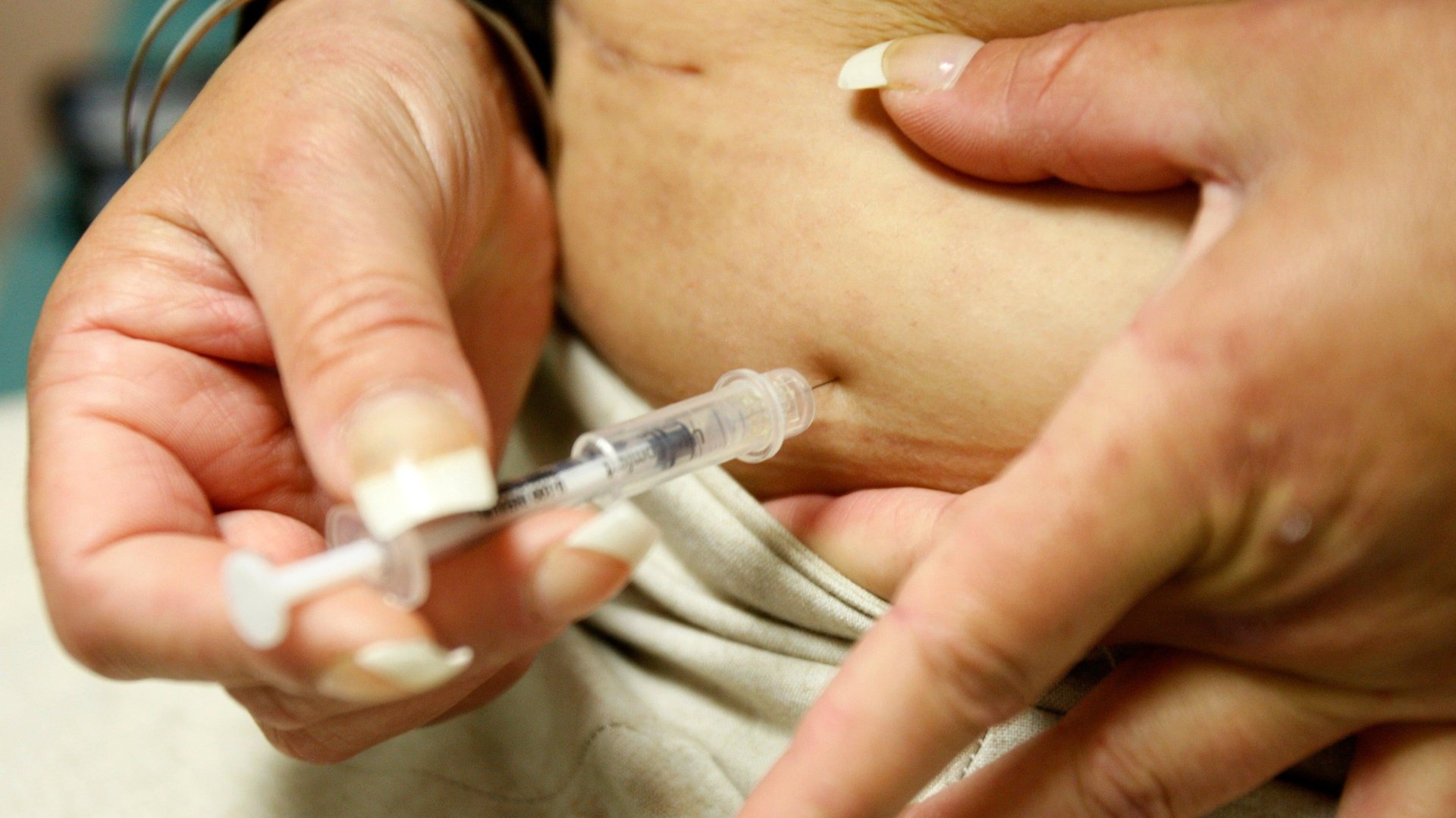
The Inflation Reduction Act of 2022 passed by the US senate on Aug. 7 was supposed to include, among other measures to lower drug costs, a cap on insulin copays for all insured patients.
But the measure, which passed the House in March, was opposed by 43 Republican senators, who eventually managed, in the Inflation Reduction legislation, to limit its application to Medicare patients only. For those insulin users, the maximum monthly co-pay will be $35, while privately insured patients may have face a higher out-of-pocket cost, depending on their insurance plan.
The Republican choice not to protect more Americans from high insulin prices will affect thousands of people. But even in its original formulation, the cap was not—as some Democrats have suggested—going to control the outrageous price of insulin in the US, nor was it offering a lifeline to the diabetic patients who suffer the most from insulin price gauging: the uninsured.
In fact, there is even a chance that failing to include private patients in the bill might maintain pressure for actual measures to control insulin prices.
The problem of insulin in the US
Insulin is an old, lifesaving medication that patients suffering from diabetes depend on to survive. The ingredients haven’t changed in decades, and estimates of the cost of production are between $3 and $5 a vial. In Canada, Europe, and many wealthy countries, the average cost per vial is under $9. In the US, it’s $113. Depending on several factors, patients might need up to six vials or more per month.
“Insulin is the poster child for what is wrong with medication prices in this country,” says Robin Feldman, a professor of law at the University of California Hastings and author of Drugs, Money, & Secret Handshakes: The Unstoppable Growth of Prescription Drug Prices. There are only a few makers of insulin in the US, she explains, and they move in lockstep—in the absence of regulations on the prices they can impose, they have more to gain by pushing them up rather than by competing for lower prices.
For some people who need insulin, prices have been so prohibitive that they have been forced to ration whatever quantities they could afford. This can be deadly, and has been; several people have died in recent years because of insulin rationing.
The government can and should put an end to this by legislating to control the price of insulin, but the bill to cap copay does the opposite of that.
A copay cap is not price cap
The limitations of an approach that limits the copay, rather than controls the price a pharmaceutical company can charge for the medication shows very clearly in the small portion of the copay cap that was maintained, limiting the maximum out-of-pocket expense for insulin to $35 for Medicare patients.
The bill caps the copay but not the price of the drug, and Medicare was notably not given authority to negotiate insulin prices. This means that Medicare will have to pick up the tab for the lowered copay, for which the bill sets aside $1.5 million, on top of other Medicare funds already already available for drug purchasing. Essentially, the excessive cost of insulin is sustained by taxpayers, not eliminated.
Similarly, if the provision was extended to privately insured patients, insurance would have to pay for the difference between the maximum copay and the cost of the drug. Premiums would go up to compensate for the additional costs, and there would continue to be absolutely no incentive for pharmaceutical companies to lower the costs of insulin.
Not only that, but such measures would only make a difference—and often a somewhat negligible one—for a minority of patients. According to analysis by KFF, a healthcare research organization, only about a quarter of insured people pay more than $35 for insulin prescription anyway. For them, the savings would be relatively small, between $19 and $42 per month for most people, and up for $71 for those purchasing insurance coverage individually.
It isn’t nothing. But it changes nothing for people who cannot afford to buy insurance, and would still have to pay up to $1,200 a month for insulin.
“By and large, the patients who are rationing insulin and have died are all uninsured—that’s the root of the problem,” says Laura Marston, who suffers from diabetes and is an advocate for lower insulin prices.
Without discounting that insured people, too, deserve reasonable prices for insulin, and that for some, paying for insulin is a real financial hardship, there is a potential silver lining to leaving them out of the copay cap.
Keeping the momentum
One thing a copay cap does well is hide drug price increases from insured patients. This is something pharmaceutical companies know well, and have taken advantage of for some time, because in most cases, the copays don’t go up dramatically even when drug prices do—although eventually subscribers see premiums go up.
If the cap had gone into effect, says Marston, there is a chance the issue of expensive insulin would have been forgotten, because the more privileged patients would have it covered for $35 or under a month. But without the provision, many more people remain invested in lower insulin prices—not controlled copays.
This could be achieved with a federal bill that set a maximum price of, say, $20 per vial of insulin (which would still be more than twice the price of most other rich countries), plus a program—ideally funded by insulin makers—to provide financial supports to patients who can’t afford the price out of pocket.
“From the perspective of wanting every person in this country who needs insulin to have it I’m not going to say we’re in a better place, but we’ve appropriately set the stage for a real insulin price cap,” says Marston.
