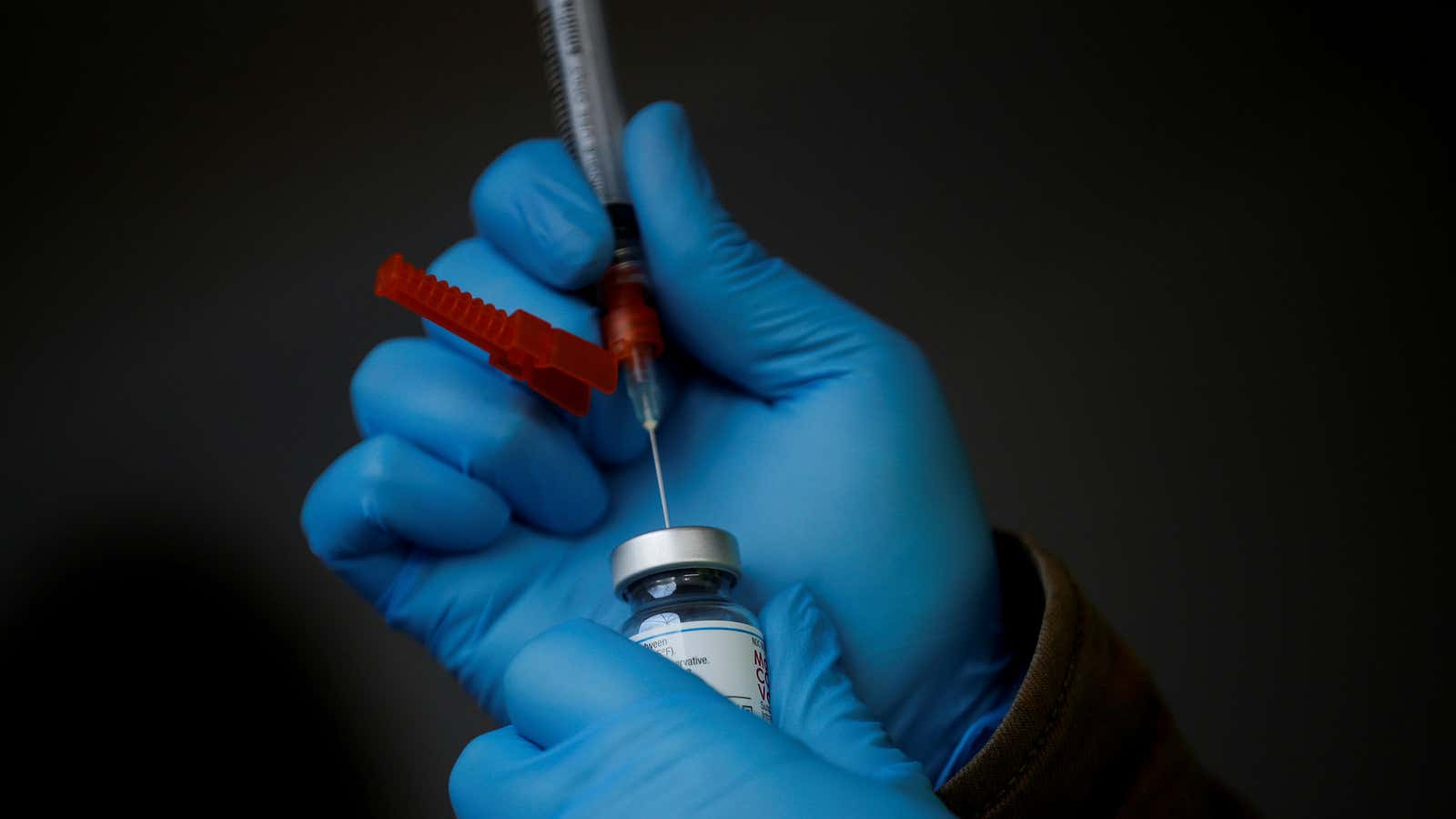
As researchers become more aware of strains of SARS-CoV-2, the virus that causes Covid-19, public health officials have one question: Will vaccines offer protection against them?
At the moment, there are two broad kinds of mutations scientists are keeping an eye on: Some that make the virus more infectious, and others that appear to make it capable of evading antibodies generated by vaccines.
These new strains are somewhat expected—viruses mutate constantly. Their only evolutionary goal is to be a glorified genetic copy-and-paste machine; destroyed cells and illness are just collateral damage. It’s understandable that sometimes, viruses make copying mistakes in their genetic code along the way—and sometimes, those bugs end up being perks for them instead.
“What’s going on now is the virus is adapting to a new host,” says David Topham, a microbiologist and immunologist at the University of Rochester in New York. SARS-CoV-2 didn’t start out as a virus infectious to humans—it began as an animal virus. Now that it’s had over a year of practice copying itself in people, it’s not surprising that it’s gotten better at replicating and surviving among us.
(More) infectious agents
The first kind of mutations scientists have noticed, which seem to make the virus more infectious, first popped up in the UK. This variant is called B.1.1.7. Now, Covid-19 cases caused by viruses with B.1.1.7 lineage have popped up in several countries including the US, where it risks becoming the dominant strain in a few months.
The B.1.1.7 variant has a slightly altered spike protein, which the virus uses like a crowbar to pry its way into our cells. It’s swapped out some of the amino-acid building blocks in previous strains for others. These exchanges, which likely occurred by chance, act like an extra grappling hook.
The overall effect of these amino acid swaps makes the virus a little better at clawing its way into our cells, says Topham. As the virus whizzes through our bodies and collides randomly with our cells, the extra grappling hook grips on just a little more tightly, increasing the chances that the virus can work its way inside. This extra stickiness means that smaller viral loads of the B.1.1.7 variant could cause an infection, which could lead to even more people becoming sick. Preliminary data suggest these strains are about 50% more infectious than previous strains.
Evading antibodies
The other strain scientists are keeping tabs on originated in Brazil. Its lineage is called P.1, and it has also traded some amino acids for others. Because the P.1 strain has been found in people who have gotten a second case of Covid-19, scientists believe that somehow, these mutations hide the virus from at least some of the protective antibodies generated by a past infection or vaccine. It’s not clear how exactly this happens just yet.
Fortunately, the cells that make antibodies, called B-cells, are fantastically responsive to change. It doesn’t matter if they learned to make antibodies against SARS-CoV-2 from a prior infection with a different strain or from a vaccine. “As long as the antibodies they express are even slightly reactive with the spike protein, they will adapt to that viral protein very quickly,” Topham says. He’s hopeful that any previous immunity to SARS-CoV-2 will still have some utility against new viral strains—even if it takes a little time to adapt.
While these mutations may sound scary, there’s at least some good news: “As far as we can tell, there’s no change in the severity of disease,” with any of these variants, Topham says. So even if these strains stick better to our cells or hide from some antibodies, the resulting illness won’t likely be worse.
And there are still ways to decrease the chances of getting sick in the first place, which major health organizations have been touting for months: Wearing a mask, keeping apart, and washing hands.