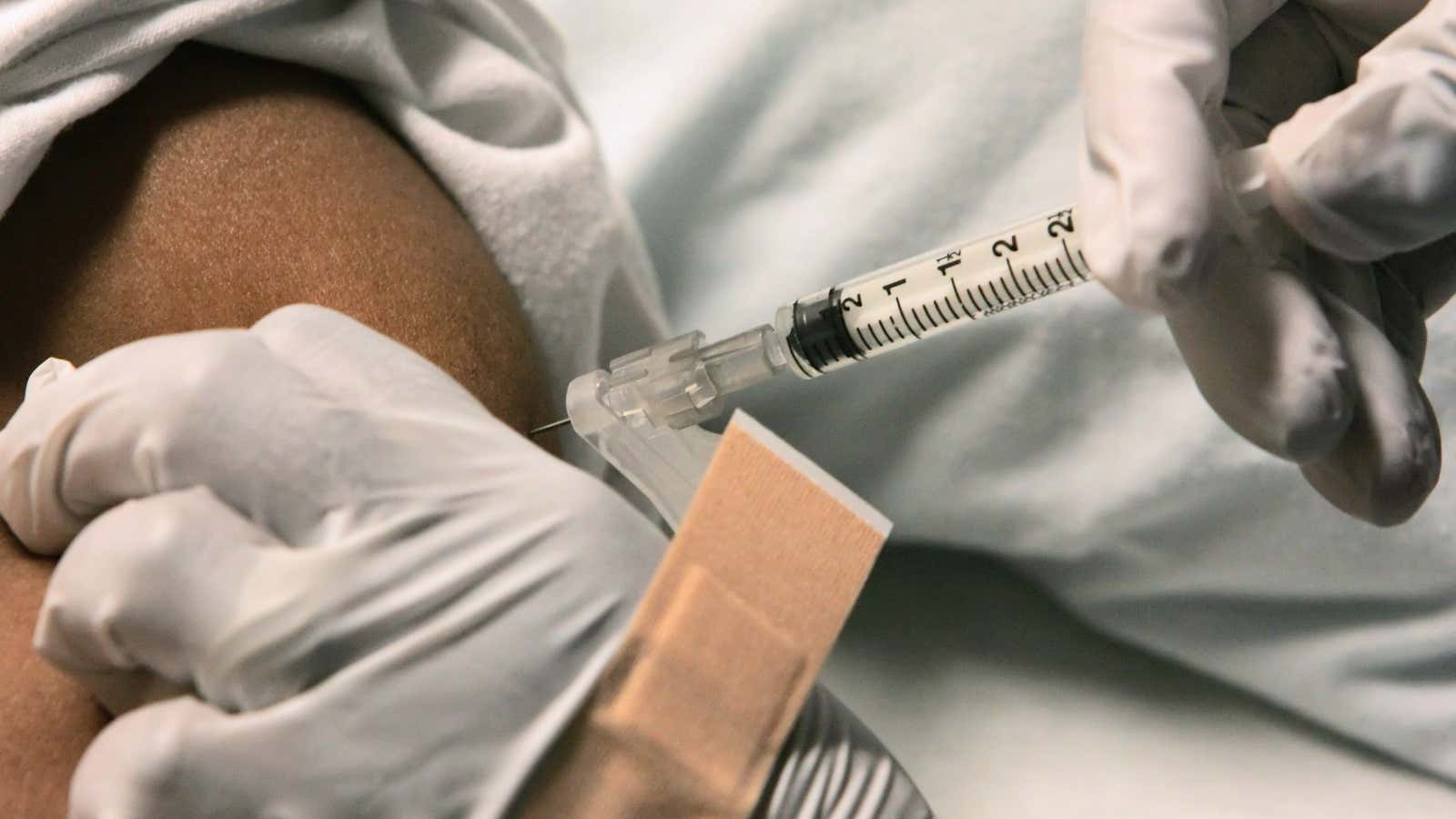
A $2, 10-minute rapid point-of-care tool has brought the much elusive goal of rapidly screening Africa’s newborns for sickle cell disease (SCD), a major cause of child mortality, within reach.
Sickle cell disease, which is also known as Sickle cell anemia, is an inherited red blood cell disorder which affects over 12 million people, mostly with origins in sub-Saharan Africa, India, Saudi Arabia and Mediterranean countries The disease is regarded as a silent baby killer as an estimated 50% to 80% of infants born with the disorder die before the age of 5 years.
Each year about 300,000 infants are born with major sickle-cell disorders—including more than 200,000 cases in Africa, according to WHO. A sickle cell patient can suffer intermittent extreme body pain commonly referred to as a “crisis” due to the “sickling” of some red blood cells.
But the integration of newborn screening into existing primary healthcare immunization programs is feasible and can rapidly be implemented with limited resources, according to a study led by professor Obiageli Nnodu, director of the Centre of Excellence for Sickle Cell Disease Research and Training at Nigeria’s University of Abuja.
Nnodu said about 10% of children in Nigeria with anemia have sickle cell disease while about 1.4% of newborns have it. But among children over the age of five, sickle cell prevalence is 0.9%, suggesting many children that were born with the disease could have died before that age..

“Most of these deaths are preventable by starting the children early on folic acid, immunization, treating malaria and administering oral penicillin. But we will not know which child requires special attention if we are not testing every newborn,” Nnodu told Quartz Africa.
Africa’s healthcare systems largely rely on a referral system for newborn screening. A baby’s blood sample is collected on a filter paper which is dispatched to a central laboratory for testing. It could take several weeks to get the result.
To realistically screen every newborn for sickle cell disease, Nnodu says a simple, reliable and affordable point-of-care rapid test will be deployed at immunization clinics, a place most newborns will visit soon after birth. One such example is the HemoTypeSC) from Silver Lake Research, a diagnostics firm based in southern California. Already registered in Nigeria, Ghana and Kenya, the test utilizes specific and sensitive monoclonal antibodies that are embedded on a test strip to detect hemoglobins A, S, and C.
“Lab tests are sub-optimal for large-scale newborn screening compared with point-of-care tests and we are already having conversations with governments and agencies that have been advocating for newborn screening,” says Erik Serrao, a vice president at the diagnostics company.
But despite recent advancements recorded in sickle cell disease, Nnodu says its end is not yet in sight considering up to 25% of the population have SCD traits and knowledge vacuums still exist. “We still have several unanswered questions including what makes one child to have a clinical course that is different from that of another child within the same family.”
Sign up to the Quartz Africa Weekly Brief here for news and analysis on African business, tech and innovation in your inbox